TSHR (thyroid stimulating hormone receptor)
2009-11-01 Carmela Iosco , Kerry J Rhoden AffiliationMedical Genetics Unit, Department of Gynaecologic, Obstetric, Pediatric Sciences, University of Bologna, Bologna, Italy
Identity
HGNC
LOCATION
14q31.1
LOCUSID
ALIAS
CHNG1,LGR3,hTSHR-I
FUSION GENES
DNA/RNA

Structure of the TSHR gene and coding sequence (CDS). Boxes represent exons numbered 1 to 10 and proportional to length, red representing the coding sequence, grey representing untranslated regions (UTR); the horizontal line joining exons represents introns, shrunk to minimal length. Positions below the CDS are numbered relative to the transcription start.
Description
Spans 190,778 bp, contains 10 exons. Kakinuma and Nagayama (2002) identified 13 exons, but most findings relate to the 10-exon pattern.
Transcription
Regulated by a TATA-less promoter containing binding sites for GABP, TTF1, CREB, ATF2, TR/RXR, SSBP and ICER.
Major transcript (TSHR isoform 1 precursor, NM_000369.2) encoded by 10 exons, transcript length 4410 bp, 2295 bp ORF, ~100 bp 5 UTR and 1.6 kb 3 UTR; the coding region spans positions 157-2451 bp, with a signal peptide at 157-216 bp, mature peptide from 217 to 2448 bp, poly-A signal at 4371-4376. Encodes the canonical protein, 764 aa.
NCBI Entrez Gene describes two alternatively spliced variants, TSHR isoform 2 precursor (NM_001018036.1) and TSHR isoform 3 precursor (NM_001142626.1). Additional transcripts are possible; according to NCBI/Aceview, there are 10 alternatively spliced variants, based upon cDNAs deposited in GenBank derived from normal and neoplastic human tissues and cell lines. There are 3 probable alternative promoters, 6 non overlapping alternative last exons and 6 validated alternative polyadenylation sites. The mRNAs appear to differ by truncation of the 5 end, truncation of the 3 end, overlapping exons with different boundaries, alternative splicing or retention of 2 introns. There is no evidence for protein expression of splice variants.
Table 1: TSHR transcript variants. *Letters refer to NCBI Aceview nomenclature as of April 2007; names in italics refer to NCBI Entrez Gene nomenclature.
Major transcript (TSHR isoform 1 precursor, NM_000369.2) encoded by 10 exons, transcript length 4410 bp, 2295 bp ORF, ~100 bp 5 UTR and 1.6 kb 3 UTR; the coding region spans positions 157-2451 bp, with a signal peptide at 157-216 bp, mature peptide from 217 to 2448 bp, poly-A signal at 4371-4376. Encodes the canonical protein, 764 aa.
NCBI Entrez Gene describes two alternatively spliced variants, TSHR isoform 2 precursor (NM_001018036.1) and TSHR isoform 3 precursor (NM_001142626.1). Additional transcripts are possible; according to NCBI/Aceview, there are 10 alternatively spliced variants, based upon cDNAs deposited in GenBank derived from normal and neoplastic human tissues and cell lines. There are 3 probable alternative promoters, 6 non overlapping alternative last exons and 6 validated alternative polyadenylation sites. The mRNAs appear to differ by truncation of the 5 end, truncation of the 3 end, overlapping exons with different boundaries, alternative splicing or retention of 2 introns. There is no evidence for protein expression of splice variants.
| Transcription variant * | Exons in CDS | mRNA | Predicted protein | Protein evidence |
| a; isoform 1 precursor | 10 | 4570 bp | 764 aa | yes |
| b; isoform 3 precursor | 9 | 1089 bp | 274 aa | no |
| c; isoform 2 precursor | 9 | 1281 bp | 253 aa | no |
| d | 8 | 1184 bp | 231 aa | no |
| e | 9 | 901 bp | 229 aa | no |
| f | 2 | 699 bp | 167 aa | no |
| g | 6 | 1018 bp | 160 aa | no |
| h | 6 | 445 bp | 141 aa | no |
| i | 3 | 561 bp | 106 aa | no |
| j-unspliced | 1 | 2541 bp | 69 aa | no |
| k | 2 | 333 bp | 57 aa | no |
Proteins
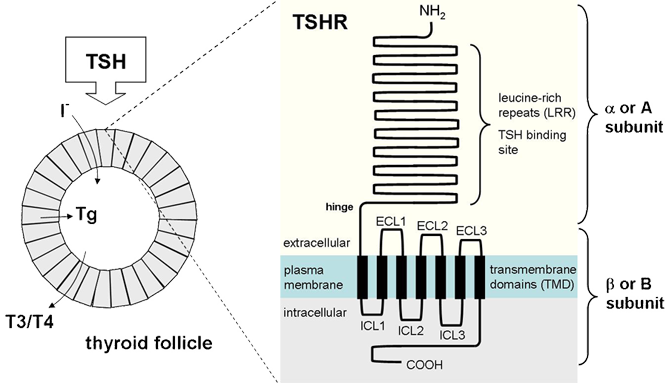
TSHR localization and structure. Left, thyroid follicle where the TSH-stimulated synthesis of thyroid hormone (T3 and T4) occurs following iodide uptake and organification into thyroglobulin (Tg). Right, TSHR protein structure, showing the A subunit composed of leucine-rich repeats (LRR) and the N-terminus, and the B subunit composed of 7 transmembrane domains (TMD), the intracellular and extracellular loops (ICL and ECL respectively) and the C-terminus.
Description
G-protein coupled receptor (GPCR), 764 aa membrane glycoprotein. Predicted MW 84.5 kDa; apparent MW of glycosylated protein 95-120 kDa.
Consists of two subunits:
(i) A or α subunit: encoded by exons 1-8 of TSHR gene; glycosylated extracellular ectodomain containing 9 leucine-rich repeats (LRR) and the N-terminus; binds TSH and other ligands (hCG and LH),
(ii) B or β subunit: encoded by exons 9-10 of TSHR gene; consists of 7 trans-membrane domains (TMD) connected by extracellular loops (important for basal and activated function) and intracellular loops (important for G protein coupling), and an intracellular C terminus.
A and B subunits are produced by posttranslational proteolytic cleavage of single-chain TSHR at the cell surface, with removal of a 50 aa peptide, and subsequent joining of A and B subunits by disulfide bridges. The B subunit is thought to be constitutionally active, and interaction with the A subunit ectodomain maintains the B subunit in an inactive state.
Consists of two subunits:
(i) A or α subunit: encoded by exons 1-8 of TSHR gene; glycosylated extracellular ectodomain containing 9 leucine-rich repeats (LRR) and the N-terminus; binds TSH and other ligands (hCG and LH),
(ii) B or β subunit: encoded by exons 9-10 of TSHR gene; consists of 7 trans-membrane domains (TMD) connected by extracellular loops (important for basal and activated function) and intracellular loops (important for G protein coupling), and an intracellular C terminus.
A and B subunits are produced by posttranslational proteolytic cleavage of single-chain TSHR at the cell surface, with removal of a 50 aa peptide, and subsequent joining of A and B subunits by disulfide bridges. The B subunit is thought to be constitutionally active, and interaction with the A subunit ectodomain maintains the B subunit in an inactive state.
Expression
Thyroid follicular epithelial cells; to a lesser degree in thymus, pituitary gland, lymphocytes, testis, retro-ocular fibroblasts, adipocytes, brain, heart and kidney.
Localisation
Plasma membrane.
Function
Regulation of thyroid metabolism.
TSHR is the receptor for thyrotropin (thyroid stimulating hormone or TSH), a member of the glycoprotein hormone family. TSH is released by the anterior pituitary gland and is the main regulator of thyroid gland growth and development. Binding of TSH to TSHR stimulates thyroid epithelial cell proliferation, and regulates the expression of differentiation markers such as thyroglobulin, thyroperoxidase and the sodium iodide symporter (NIS), necessary for the synthesis of thyroid hormones.
TSHR is coupled to heterotrimetric G proteins, regulatory proteins associated with the inner surface of the plasma membrane. Binding of TSH to TSHR causes a conformational change in TSHR, provoking the GTP-dependent dissociation of the Gα subunit from GβGγ dimers. Gα activates distinct signal transduction pathways to stimulate gene transcription and cell proliferation.
Two G protein-dependent pathways are activated by TSHR:
(i) Gαs activates adenylate cyclase to increase cAMP levels; cAMP activates protein kinase A (PKA) causing translocation of its catalytic subunit to the nucleus; PKA phosphorylates, among others, the transcription factor CREB thereby increasing its transcriptional activity.
(ii) Gαq activates phospholipase C to increase phosphoinositide turnover, releasing inositol triphosphate (IP3) and diacylglycerol (DAG); DAG activates protein kinase C, which promotes proliferation via the RAF/MEK/ERK pathway.
Complex cross-talk occurs between these pathways and other signaling pathways including the PI3/Akt, PKC/NFkB and JAK/STAT pathways (for reviews see García-Jiménez and Santisteban (2007) and Latif et al. (2009)).
TSHR is also activated by other members of the glycoprotein hormone family, including human chorionic gonadotropin (hCG), luteinizing hormone (LH) and thyrostimulin (a heterodimer composed of A2 and B5 glycoprotein hormone subunits).
TSHR is the receptor for thyrotropin (thyroid stimulating hormone or TSH), a member of the glycoprotein hormone family. TSH is released by the anterior pituitary gland and is the main regulator of thyroid gland growth and development. Binding of TSH to TSHR stimulates thyroid epithelial cell proliferation, and regulates the expression of differentiation markers such as thyroglobulin, thyroperoxidase and the sodium iodide symporter (NIS), necessary for the synthesis of thyroid hormones.
TSHR is coupled to heterotrimetric G proteins, regulatory proteins associated with the inner surface of the plasma membrane. Binding of TSH to TSHR causes a conformational change in TSHR, provoking the GTP-dependent dissociation of the Gα subunit from GβGγ dimers. Gα activates distinct signal transduction pathways to stimulate gene transcription and cell proliferation.
Two G protein-dependent pathways are activated by TSHR:
(i) Gαs activates adenylate cyclase to increase cAMP levels; cAMP activates protein kinase A (PKA) causing translocation of its catalytic subunit to the nucleus; PKA phosphorylates, among others, the transcription factor CREB thereby increasing its transcriptional activity.
(ii) Gαq activates phospholipase C to increase phosphoinositide turnover, releasing inositol triphosphate (IP3) and diacylglycerol (DAG); DAG activates protein kinase C, which promotes proliferation via the RAF/MEK/ERK pathway.
Complex cross-talk occurs between these pathways and other signaling pathways including the PI3/Akt, PKC/NFkB and JAK/STAT pathways (for reviews see García-Jiménez and Santisteban (2007) and Latif et al. (2009)).
TSHR is also activated by other members of the glycoprotein hormone family, including human chorionic gonadotropin (hCG), luteinizing hormone (LH) and thyrostimulin (a heterodimer composed of A2 and B5 glycoprotein hormone subunits).
Mutations
Note
Over 90 naturally occurring TSHR mutations have been identified, and are catalogued in the GRIS database and TSHR mutation database. Mutations are gain-of-function resulting in constitutional activation of the receptor independently of TSH, or loss-of-function resulting in loss of TSH sensitivity.
Polymorphisms: Coding missense SNPs: Pro27Thr, Glu34Lys, Asp36His, Pro52Thr, Thr574Ser, Tyr601His, Val721Phe, Glu727Asp, Asn 744Lys.
Polymorphisms: Coding missense SNPs: Pro27Thr, Glu34Lys, Asp36His, Pro52Thr, Thr574Ser, Tyr601His, Val721Phe, Glu727Asp, Asn 744Lys.
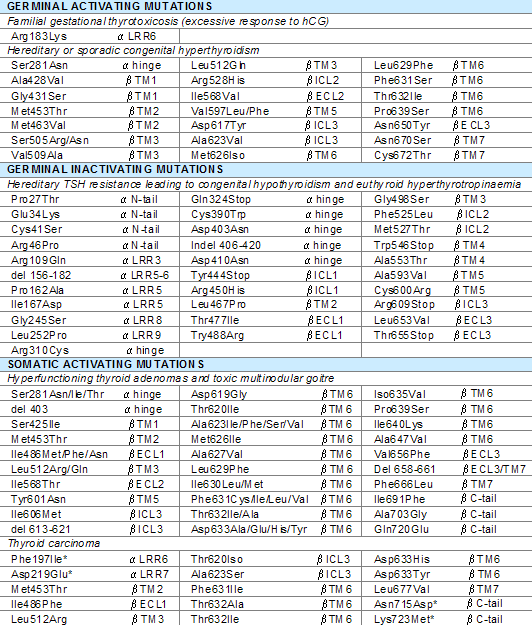
Table 2: TSHR mutations in thyroid disease. Mutations are listed in terms of the amino acid residues altered and their respective location (α = A subunit, β = B subunit, TM = transmembrane domain, ICL = intracellular loop, ECL = extracellular loop, LRR = leucine-rich repeat, hinge = domain connecting leucine-rich repeats to first transmembrane domain).
Note: * unknown functional status of mutations (Ohno et al., 1995).
Germinal
Germinal TSHR mutations include missense mutations, nonsense mutations, insertion/deletions, and exon skipping due to alternative splicing. Germinal activating mutations are associated with hereditary or sporadic congenital hyperthyroidism, whereas germinal inactivating mutations are a cause of TSH resistance associated with congenital hypothyroidism and euthyroid hyperthyrotropinaemia.
Somatic
Somatic TSHR mutations include missense mutations and in-frame deletions. Activating mutations have been identified in hyperfunctioning thyroid adenoma and toxic multinodular goiter; few cases are associated with thyroid carcinoma. No somatic inactivating mutations have been described so far.
Implicated in
Entity name
Thyroid adenoma
Disease
Somatic activating TSHR mutations are a major cause of hyperfunctioning thyroid adenomas, benign neoplasms of thyroid follicular cells:
- 10-80% of hyperfunctioning or hot adenomas (i.e. ademomas with active radioiodide uptake and thyroid hormone synthesis) harbor somatic activating mutations (Parma et al., 1993; Russo et al., 1996; Führer et al., 2007). The highly variable frequency of mutations may reflect geographic differences.
- Activating mutations are largely located in exon 10 encoding the TSHR β-subunit, and are particularly frequent in the sixth transmembrane segment (TM6) important for coupling to G proteins.
- Mutations result in the constitutive activation of adenylate cyclase, stimulating thyrocyte proliferation and thyroid hormone synthesis. As a consequence, hyperfunctioning nodules provoke hyperthyroidism and thyrotoxicosis.
- Nonfunctioning or cold adenomas (i.e. not able to accumulate radioiodide or synthesize thyroid hormones) do not harbor TSHR mutations.
- 10-80% of hyperfunctioning or hot adenomas (i.e. ademomas with active radioiodide uptake and thyroid hormone synthesis) harbor somatic activating mutations (Parma et al., 1993; Russo et al., 1996; Führer et al., 2007). The highly variable frequency of mutations may reflect geographic differences.
- Activating mutations are largely located in exon 10 encoding the TSHR β-subunit, and are particularly frequent in the sixth transmembrane segment (TM6) important for coupling to G proteins.
- Mutations result in the constitutive activation of adenylate cyclase, stimulating thyrocyte proliferation and thyroid hormone synthesis. As a consequence, hyperfunctioning nodules provoke hyperthyroidism and thyrotoxicosis.
- Nonfunctioning or cold adenomas (i.e. not able to accumulate radioiodide or synthesize thyroid hormones) do not harbor TSHR mutations.
Entity name
Toxic multinodular goiter (Plummers disease)
Disease
Somatic activating TSHR mutations are a major cause of Toxic Multinodular Goiter (TMNG), a hyperplastic thyroid enlargement with multiple bilateral nodules:
- 70-80% of hyperfunctioning nodules of TMNG harbor somatic activating mutations, many of which are shared with hyperfunctioning thyroid adenoma suggesting a common pathogenic event (Tonacchera et al., 1998; Tonacchera et al., 2000).
- Different hyperfunctioning nodules within a goiter harbor may distinct TSHR activating mutations, confirming the polyclonal etiology of TMNG. In contrast, nonfunctioning nodules within the same goiter do not harbor mutations.
- TMNG is most common in iodine-deficient areas, and this may reflect the increased mutagenic load associated with chronic TSH stimulation and thyrocyte proliferation.
- A germline polymorphism of codon 727 of TSHR was reported to be associated with TMNG (Gabriel et al., 1999), however a subsequent study failed to substantiate this finding in a European population (Mulhberg et al., 2000).
- 70-80% of hyperfunctioning nodules of TMNG harbor somatic activating mutations, many of which are shared with hyperfunctioning thyroid adenoma suggesting a common pathogenic event (Tonacchera et al., 1998; Tonacchera et al., 2000).
- Different hyperfunctioning nodules within a goiter harbor may distinct TSHR activating mutations, confirming the polyclonal etiology of TMNG. In contrast, nonfunctioning nodules within the same goiter do not harbor mutations.
- TMNG is most common in iodine-deficient areas, and this may reflect the increased mutagenic load associated with chronic TSH stimulation and thyrocyte proliferation.
- A germline polymorphism of codon 727 of TSHR was reported to be associated with TMNG (Gabriel et al., 1999), however a subsequent study failed to substantiate this finding in a European population (Mulhberg et al., 2000).
Entity name
Thyroid carcinoma
Prognosis
TSHR mRNA in thyroid tumours: Reduced or absent TSHR mRNA in thyroid tumours is a negative prognostic marker, indicative of reduced effectiveness of radioiodine therapy. TSHR expression in thyroid carcinoma correlates with the state of differentiation of tumours, with loss of differentiation resulting in a loss of mRNA expression. Thus, well-differentiated carcinomas (papillary and follicular) show variable TSHR mRNA levels ranging from normal to markedly reduced, whereas undifferentiated anaplastic carcinoma shows absent TSHR mRNA (Brabant et al., 2001; Brönnegård et al., 1994; Shiels et al., 1999). TSHR regulates the thyroid expression of the iodide transporter NIS, and decreased TSHR expression impairs the iodine-concentrating capacity of thyroid tumours.
Circulating TSHR mRNA: TSHR mRNA in peripheral blood has been suggested as a potential molecular marker of circulating thyroid carcinoma cells to aid in the differential diagnosis of malignant and benign thyroid disease preoperatively, and to detect residual, recurrent or metastatic thyroid cancer (Barzon et al., 2004; Chinnappa et al., 2004).
TSHR promoter methylation: TSHR promoter methylation may be a marker for malignancy in thyroid carcinoma (Xing et al., 2003).
Circulating TSHR mRNA: TSHR mRNA in peripheral blood has been suggested as a potential molecular marker of circulating thyroid carcinoma cells to aid in the differential diagnosis of malignant and benign thyroid disease preoperatively, and to detect residual, recurrent or metastatic thyroid cancer (Barzon et al., 2004; Chinnappa et al., 2004).
TSHR promoter methylation: TSHR promoter methylation may be a marker for malignancy in thyroid carcinoma (Xing et al., 2003).
Oncogenesis
TSHR mutations: Mutagenic screening of thyroid carcinomas reveals a low incidence of somatic TSHR mutations ranging from 0-22%, suggesting a limited role for TSHR mutations in the pathogenesis of thyroid carcinoma (Matsuo et al., 1993; Russo et al., 1995; Ohno et al., 1995; Spambalg et al., 1996; Esapa et al., 1997; Cetani et al., 1999).
- Thr632Ile in thyroid hormone-producing follicular carcinoma (Spambalg et al., 1996).
Rare cases of TSHR mutations in nonfunctioning thyroid carcinoma have also been reported:
- Ile486Phe in an autonomously functioning follicular carcinoma presenting a hot nodule causing hyperthyroidism (Camacho et al., 2000).
- Leu512Arg in autonomously functioning papillary carcinoma with hot nodule (Gozu et al., 2004).
- Leu677Val in autonomously functioning Hürthle cell thyroid carcinoma causing thyrotoxicosis (Russo et al., 1999).
- Phe631Ile and Asp633Tyr in toxic metastasizing follicular thyroid carcinoma; no TSHR mutations in non-functioning lung metastases (Führer et al., 2003).
- Asp633His in aggressive insular thyroid carcinoma (poorly-differentiated carcinoma) presenting as an autonomously functioning thyroid nodule and causing severe thyrotoxicosis; TSHR mutation also present in lymph node metastasis (Russo et al., 1997).
- Thr632Ala in nonfunctioning follicular carcinoma (Spambalg et al., 1996).
- Ala623Ser activating mutation in papillary carcinoma with cold nodule, in patient with past history of Graves disease (De Cross et al., 2008).
The role of activating TSHR mutations in neoplastic transformation is unclear. Although TSHR activation stimulates thyrocyte proliferation, hyperfunctioning nodules (adenoma or toxic multinodular goiter) are rarely malignant, suggesting that constitutive activation of the cAMP cascade alone is insufficient for the malignant transformation of thyroid follicular cells.
Epigenetics: The TSHR gene promoter is frequently hypermethylated in thyroid carcinoma, with preferential methylation in undifferentiated carcinoma (Xing et al., 2003; Schagdarsurengin et al., 2006). In contrast, TSHR gene promoter is unmethylated in the normal thyroid and in benign tumours (thyroid adenoma). Hypermethylation results in TSHR gene silencing and reduced TSHR expression in some malignant thyroid tumours. In thyroid cancer cell lines, demethylating agents partially restore TSHR expression.
- Thr632Ile in thyroid hormone-producing follicular carcinoma (Spambalg et al., 1996).
Rare cases of TSHR mutations in nonfunctioning thyroid carcinoma have also been reported:
- Ile486Phe in an autonomously functioning follicular carcinoma presenting a hot nodule causing hyperthyroidism (Camacho et al., 2000).
- Leu512Arg in autonomously functioning papillary carcinoma with hot nodule (Gozu et al., 2004).
- Leu677Val in autonomously functioning Hürthle cell thyroid carcinoma causing thyrotoxicosis (Russo et al., 1999).
- Phe631Ile and Asp633Tyr in toxic metastasizing follicular thyroid carcinoma; no TSHR mutations in non-functioning lung metastases (Führer et al., 2003).
- Asp633His in aggressive insular thyroid carcinoma (poorly-differentiated carcinoma) presenting as an autonomously functioning thyroid nodule and causing severe thyrotoxicosis; TSHR mutation also present in lymph node metastasis (Russo et al., 1997).
- Thr632Ala in nonfunctioning follicular carcinoma (Spambalg et al., 1996).
- Ala623Ser activating mutation in papillary carcinoma with cold nodule, in patient with past history of Graves disease (De Cross et al., 2008).
The role of activating TSHR mutations in neoplastic transformation is unclear. Although TSHR activation stimulates thyrocyte proliferation, hyperfunctioning nodules (adenoma or toxic multinodular goiter) are rarely malignant, suggesting that constitutive activation of the cAMP cascade alone is insufficient for the malignant transformation of thyroid follicular cells.
Epigenetics: The TSHR gene promoter is frequently hypermethylated in thyroid carcinoma, with preferential methylation in undifferentiated carcinoma (Xing et al., 2003; Schagdarsurengin et al., 2006). In contrast, TSHR gene promoter is unmethylated in the normal thyroid and in benign tumours (thyroid adenoma). Hypermethylation results in TSHR gene silencing and reduced TSHR expression in some malignant thyroid tumours. In thyroid cancer cell lines, demethylating agents partially restore TSHR expression.
Entity name
Congenital nongoitrous hypothyroidism-1 (CHNG1)
Disease
Germline inactivation TSHR mutations are a cause of hereditary congenital nongoitrous hypothyroidism. Inactivating mutations result in variable degrees of TSH resistance, with clinical consequences ranging from euthyroid hyperthyrotropinemia to mild or severe hypothyroidism. CHNG1 is inherited in an autosomal recessive manner, manifesting in homozygotes or compound heterozygotes. However, subclinical hypothyroidism may also manifest in heterozygotes, suggesting autosomal dominant inheritance.
Entity name
Hereditary nonautoimmune hyperthyroidism
Disease
Germline activating TSHR mutations are a cause of hereditary nonautoimmune congenital hyperthyroidism (autosomal dominant inheritance). Sporadic cases of nonautoimmune congenital hyperthyroidism result from de novo germinal mutations. Activating germline mutations result in constitutive activation of the cAMP pathway in thyrocytes. Mutations are predominantly in exon 10 encoding the transmembrane domains. One activating mutation (Arg183Lys) increases sensitivity towards hCG and manifests in women during pregnancy (familial gestational hyperthyroidism).
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 15170676 | 2004 | Evaluation of circulating thyroid-specific transcripts as markers of thyroid cancer relapse. | Barzon L et al |
| 1761161 | 1991 | Human thyrotropin receptor gene: expression in thyroid tumors and correlation to markers of thyroid differentiation and dedifferentiation. | Brabant G et al |
| 8045952 | 1994 | Expression of thyrotropin receptor and thyroid hormone receptor messenger ribonucleic acid in normal, hyperplastic, and neoplastic human thyroid tissue. | Brönnegård M et al |
| 11128715 | 2000 | A Phe 486 thyrotropin receptor mutation in an autonomously functioning follicular carcinoma that was causing hyperthyroidism. | Camacho P et al |
| 10342361 | 1999 | Genetic analysis of the TSH receptor gene in differentiated human thyroid carcinomas. | Cetani F et al |
| 17118994 | 2007 | Thyroid-stimulating hormone receptor messenger ribonucleic acid measurement in blood as a marker for circulating thyroid cancer cells and its role in the preoperative diagnosis of thyroid cancer. | Chia SY et al |
| 15292293 | 2004 | Detection of thyrotropin-receptor messenger ribonucleic acid (mRNA) and thyroglobulin mRNA transcripts in peripheral blood of patients with thyroid disease: sensitive and specific markers for thyroid cancer. | Chinnappa P et al |
| 16075037 | 2005 | Thyrotropin receptor-associated diseases: from adenomata to Graves disease. | Davies TF et al |
| 18727713 | 2009 | Functional studies of new TSH receptor (TSHr) mutations identified in patients affected by hypothyroidism or isolated hyperthyrotrophinaemia. | De Marco G et al |
| 9024242 | 1997 | G protein and thyrotropin receptor mutations in thyroid neoplasia. | Esapa C et al |
| 9360556 | 1997 | Somatic mutations in the thyrotropin receptor gene and not in the Gs alpha protein gene in 31 toxic thyroid nodules. | Führer D et al |
| 14713269 | 2003 | Two somatic TSH receptor mutations in a patient with toxic metastasising follicular thyroid carcinoma and non-functional lung metastases. | Führer D et al |
| 10487707 | 1999 | Germline polymorphism of codon 727 of human thyroid-stimulating hormone receptor is associated with toxic multinodular goiter. | Gabriel EM et al |
| 17891229 | 2007 | TSH signalling and cancer. | García-Jiménez C et al |
| 15671779 | 2004 | Does a Leu 512 Arg thyrotropin receptor mutation cause an autonomously functioning papillary carcinoma? | Gozu H et al |
| 12081236 | 2002 | Multiple messenger ribonucleic acid transcripts and revised gene organization of the human TSH receptor. | Kakinuma A et al |
| 19328414 | 2009 | The thyroid-stimulating hormone receptor: impact of thyroid-stimulating hormone and thyroid-stimulating hormone receptor antibodies on multimerization, cleavage, and signaling. | Latif R et al |
| 19826830 | 2010 | United detection GNAS and TSHR mutations in subclinical toxic multinodular goiter. | Liu C et al |
| 8501149 | 1993 | The thyrotropin receptor (TSH-R) is not an oncogene for thyroid tumors: structural studies of the TSH-R and the alpha-subunit of Gs in human thyroid neoplasms. | Matsuo K et al |
| 19015922 | 2009 | Effectiveness of peripheral thyrotropin receptor mRNA in follow-up of differentiated thyroid cancer. | Milas M et al |
| 11035845 | 2000 | Hyperfunctioning malignant thyroid nodule in an 11-year-old girl: pathologic and molecular studies. | Mircescu H et al |
| 15012610 | 2004 | Decreased expression of thyrotropin receptor gene suggests a high-risk subgroup for oncocytic adenoma. | Mirebeau-Prunier D et al |
| 10946859 | 2000 | Lack of association of nonautoimmune hyperfunctioning thyroid disorders and a germline polymorphism of codon 727 of the human thyrotropin receptor in a European Caucasian population. | Mühlberg T et al |
| 16756473 | 2006 | Follicular carcinoma presenting as autonomous functioning thyroid nodule and containing an activating mutation of the TSH receptor (T620I) and a mutation of the Ki-RAS (G12C) genes. | Niepomniszcze H et al |
| 7647578 | 1995 | Point mutations in the thyrotropin receptor in human thyroid tumors. | Ohno M et al |
| 8413627 | 1993 | Somatic mutations in the thyrotropin receptor gene cause hyperfunctioning thyroid adenomas. | Parma J et al |
| 8636365 | 1996 | Thyrotropin receptor gene alterations in thyroid hyperfunctioning adenomas. | Russo D et al |
| 9062474 | 1997 | Detection of an activating mutation of the thyrotropin receptor in a case of an autonomously hyperfunctioning thyroid insular carcinoma. | Russo D et al |
| 10037070 | 1999 | A Val 677 activating mutation of the thyrotropin receptor in a Hürthle cell thyroid carcinoma associated with thyrotoxicosis. | Russo D et al |
| 16889486 | 2006 | CpG island methylation of tumor-related promoters occurs preferentially in undifferentiated carcinoma. | Schagdarsurengin U et al |
| 10398146 | 1999 | TSH receptor status of thyroid neoplasms--TaqMan RT-PCR analysis of archival material. | Sheils OM et al |
| 17938324 | 2007 | Methylation status of genes in papillary thyroid carcinoma. | Smith JA et al |
| 8923835 | 1996 | Structural studies of the thyrotropin receptor and Gs alpha in human thyroid cancers: low prevalence of mutations predicts infrequent involvement in malignant transformation. | Spambalg D et al |
| 10852462 | 2000 | Activating thyrotropin receptor mutations are present in nonadenomatous hyperfunctioning nodules of toxic or autonomous multinodular goiter. | Tonacchera M et al |
| 16543405 | 2006 | GRIS: glycoprotein-hormone receptor information system. | Van Durme J et al |
| 12727856 | 2003 | Methylation of the thyroid-stimulating hormone receptor gene in epithelial thyroid tumors: a marker of malignancy and a cause of gene silencing. | Xing M et al |
| 19082310 | 2008 | Fatal outcome of a young woman with papillary thyroid carcinoma and graves' disease: possible implication of "cross-signalling" mechanism. | Cross GA et al |
Other Information
Locus ID:
NCBI: 7253
MIM: 603372
HGNC: 12373
Ensembl: ENSG00000165409
Variants:
dbSNP: 7253
ClinVar: 7253
TCGA: ENSG00000165409
COSMIC: TSHR
RNA/Proteins
Expression (GTEx)
Pathways
Protein levels (Protein atlas)
References
| Pubmed ID | Year | Title | Citations |
|---|---|---|---|
| 38194289 | 2024 | Mechanisms of thyrotropin receptor-mediated phenotype variability deciphered by gene mutations and M453T-knockin model. | 0 |
| 38433572 | 2024 | TSHR Variant Screening and Phenotype Analysis in 367 Chinese Patients With Congenital Hypothyroidism. | 0 |
| 38566871 | 2024 | A Novel TSHR Gene Mutation in a Family with Non-autoimmune Hyperthyroidism. | 0 |
| 38194289 | 2024 | Mechanisms of thyrotropin receptor-mediated phenotype variability deciphered by gene mutations and M453T-knockin model. | 0 |
| 38433572 | 2024 | TSHR Variant Screening and Phenotype Analysis in 367 Chinese Patients With Congenital Hypothyroidism. | 0 |
| 38566871 | 2024 | A Novel TSHR Gene Mutation in a Family with Non-autoimmune Hyperthyroidism. | 0 |
| 36842079 | 2023 | [Pathogenic TSHR variants in children with thyroid dysgenesis]. | 0 |
| 37042127 | 2023 | Unraveling the significance of TSHR mutations in indeterminate thyroid cytology specimens. | 0 |
| 37346832 | 2023 | Eighteen-years follow-up of congenital hypothyroidism by TSHR gene p.Arg109Gln and p.Arg450His variants. | 0 |
| 37561783 | 2023 | Molecular investigation of TSHR gene in Bangladeshi congenital hypothyroid patients. | 2 |
| 37716507 | 2023 | Somatostatin Receptor Type 2 and Thyroid-Stimulating Hormone Receptor Expression in Oncocytic Thyroid Neoplasms: Implications for Prognosis and Treatment. | 0 |
| 36842079 | 2023 | [Pathogenic TSHR variants in children with thyroid dysgenesis]. | 0 |
| 37042127 | 2023 | Unraveling the significance of TSHR mutations in indeterminate thyroid cytology specimens. | 0 |
| 37346832 | 2023 | Eighteen-years follow-up of congenital hypothyroidism by TSHR gene p.Arg109Gln and p.Arg450His variants. | 0 |
| 37561783 | 2023 | Molecular investigation of TSHR gene in Bangladeshi congenital hypothyroid patients. | 2 |
Citation
Carmela Iosco ; Kerry J Rhoden
TSHR (thyroid stimulating hormone receptor)
Atlas Genet Cytogenet Oncol Haematol. 2009-11-01
Online version: http://atlasgeneticsoncology.org/gene/290/tshr
