Bone: Dedifferentiated chondrosarcoma
2012-03-01 Andreas F Mavrogenis , Panayiotis J Papagelopoulos Affiliation1.First Department of Orthopaedics, Athens University Medical School, ATTIKON University Hospital, Athens, Greece
Summary
Note
Dedifferentiated chondrosarcoma was first proposed in 1971 by Dahlin and Beabout. It is characterized by two distinct histopathological components; a well-differentiated benign chondral lesion or chondrosarcoma (any grade) sharply juxtaposed with a high-grade non-cartilaginous component; typically there is an abrupt transition between the two tissue types. The non-cartilaginous component of dedifferentiated chondrosarcoma is generally an osteosarcoma, a fibrosarcoma, or a malignant fibrous histiocytoma. Dedifferentiation to leiomyosarcoma, giant cell tumor, and rarely, clear-cell chondrosarcoma or rhabdomyosarcoma has been reported.
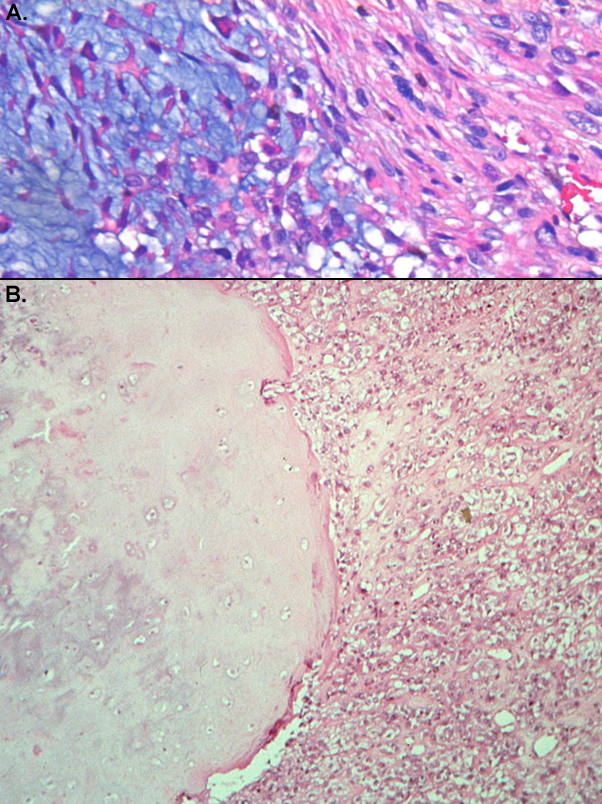
A. Photomicrograph (stain, hematoxylin and eosin; original magnification, 10x) shows abrupt transition between a low grade chondrosarcoma (left) and a high grade spindle cell sarcoma (right). B. Photomicrograph (stain, hematoxylin and eosin; original magnification, 2x) shows abrupt transition between a low grade chondrosarcoma (left) and a high grade spindle cell sarcoma (right).
Clinics and Pathology
Note
Pathogenesis unclear. Dahlin and Beabout suggested that dedifferentiation is the result of direct transformation of a well-differentiated cartilage lesion, while others suggested that it is related to transformation within the dense fibrotic reaction surrounding necrotic areas at the margin of the chondral component by a process analogous to the development of fibrosarcomas in bone infarcts and chronic osteomyelitis. Others advocate that dedifferentiation is the result of two differing clones of cells, one of which differentiates into a low-grade chondrosarcoma, while the other fails to differentiate and displays features of a high-grade sarcoma.
Epidemiology
Dedifferentiated chondrosarcoma accounts for approximately 10% of all chondrosarcomas and shows an increased growth rate and rapid metastatic spread in comparison with ordinary chondrosarcomas. It arises most frequently in the 5th and 6th decade of life. Anatomically, the femur, pelvis and humerus are the most common sites of involvement.
Clinics
Clinical symptoms include pain, swelling, palpable tumor masses and a high rate (30%) of pathological fractures. Approximately 20% of patients have metastases at diagnosis.
Radiographically, dedifferentiation is suggested by a sharply demarcated area of aggressive bone destruction associated with an underlying cartilaginous lesion and the presence of an extraosseous soft-tissue mass. Three radiographic types of dedifferentiated chondrosarcoma have been described. In type 1, the radiographic appearance is the same as for a central chondrosarcoma, with the addition of a region with very aggressive bone destruction. In type 2, lesions resemble an underlying benign enchondroma but also have destructive changes and/or a large soft tissue mass. In type 3, lesions are not distinctive radiographically and present as a very high-grade destructive lesion of bone.
The dedifferentiated component can easily be detected by MRI, as a sharply defined osteolytic area of reduced signal intensity adjacent to the hyperintense chondral component corresponding to regions of dedifferentiation. Three distinct MRI patterns have been described. In the first, there is clear demarcation between the two regions of high and reduced T2-weighted signal intensity, a so-called biphasic pattern. This pattern typically correlates with a type 1 radiographic lesion. In the second pattern, the only MRI evidence of an underlying chondral lesion is the presence of multiple areas of signal void corresponding to matrix mineralization identified radiographically; this indicates the presence of underlying or residual enchondromas, and correlates with a type 2 radiographic lesion. In the third MRI pattern, the vast majority of the lesion has a relatively reduced signal intensity compared with typical chondral tissue and a diagnosis of an underlying chondral component could not be made on MRI. In this case, smaller areas of hyperintensity on T2-weighted images could be seen within the main tumor mass. These presumably correspond to tumor necrosis rather than chondral tissue, and correlate with a type 3 radiographic lesion.
Radiographically, dedifferentiation is suggested by a sharply demarcated area of aggressive bone destruction associated with an underlying cartilaginous lesion and the presence of an extraosseous soft-tissue mass. Three radiographic types of dedifferentiated chondrosarcoma have been described. In type 1, the radiographic appearance is the same as for a central chondrosarcoma, with the addition of a region with very aggressive bone destruction. In type 2, lesions resemble an underlying benign enchondroma but also have destructive changes and/or a large soft tissue mass. In type 3, lesions are not distinctive radiographically and present as a very high-grade destructive lesion of bone.
The dedifferentiated component can easily be detected by MRI, as a sharply defined osteolytic area of reduced signal intensity adjacent to the hyperintense chondral component corresponding to regions of dedifferentiation. Three distinct MRI patterns have been described. In the first, there is clear demarcation between the two regions of high and reduced T2-weighted signal intensity, a so-called biphasic pattern. This pattern typically correlates with a type 1 radiographic lesion. In the second pattern, the only MRI evidence of an underlying chondral lesion is the presence of multiple areas of signal void corresponding to matrix mineralization identified radiographically; this indicates the presence of underlying or residual enchondromas, and correlates with a type 2 radiographic lesion. In the third MRI pattern, the vast majority of the lesion has a relatively reduced signal intensity compared with typical chondral tissue and a diagnosis of an underlying chondral component could not be made on MRI. In this case, smaller areas of hyperintensity on T2-weighted images could be seen within the main tumor mass. These presumably correspond to tumor necrosis rather than chondral tissue, and correlate with a type 3 radiographic lesion.
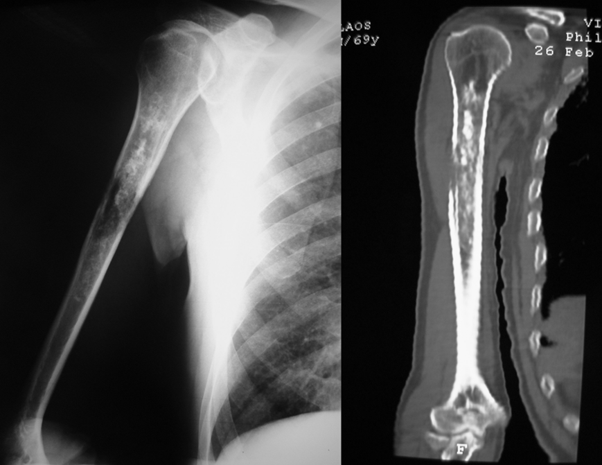
Radiograph (left) and CT (right) show osteolysis and destruction of the cortex of the humeral diaphysis of a 60-year-old man with a known enchondroma of the humerus.
Pathology
Macroscopically, both cartilaginous and noncartilaginous tumor components, typically, are grossly evident in varying proportions. The blue-grey lobulated low grade cartilaginous component is usually located centrally, while the overgrowth and expanded fleshy or haemorrhagic higher grade component is predominantly extraosseous. Microscopically, there is abrupt demarcation between the two components.
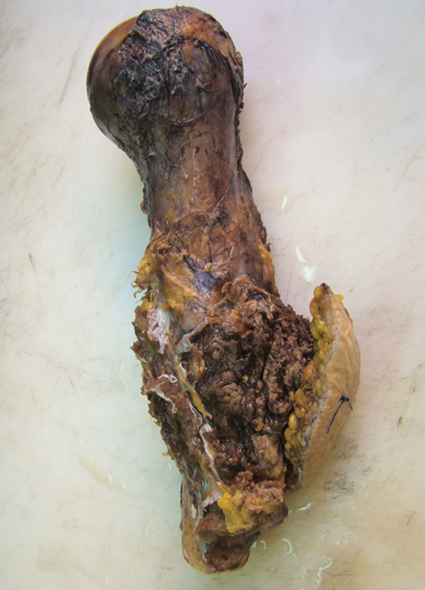
Tumor specimen after en bloc resection of the proximal humerus.
Treatment
Surgical: Chondrosarcomas are a surgical disease. High grade (grade 2 and 3) and dedifferentiated chondrosarcomas should be managed with wide resection. Chondrosarcomas of the pelvis and spine can be particularly difficult to treat due on the size of the tumor and its relationship to important adjacent structures such as the bladder or spinal cord; intralesional or marginal resection margins, and local recurrences are the highest in this group of patients with axial tumors.
Non-surgical: The role of chemotherapy remains unclear. A poor 5-year survival and no difference in overall survival between patients managed with surgery alone (11.8%) and those managed with a combination of surgery and chemotherapy (4%) has been reported. Others recommended immediate surgical removal of the lesions and postoperative chemotherapy if possible to prevent metastatic spread of the disease. Given the poor prognosis of patients with dedifferentiated chondrosarcoma, National Comprehensive Cancer Network (NCCN) guidelines suggest treating dedifferentiated chondrosarcoma in a fashion similar to osteosarcoma. Radiation therapy can be considered (1) after incomplete resection, aiming at maximal local control (curative), (2) if resection is not feasible or would cause major morbidity (palliative).
Targeted treatments: A phase II trial investigates the use of perifosine, a modulator of membrane permeability, in patients with chemotherapy insensitive tumors including chondrosarcomas. Novel anti-folates, such as pemetrexed, are currently under active investigation in patients with chondrosarcoma, as is the combination of gemcitabine and docetaxel. Finally, small-molecule inhibitors, such as dasatinib, and monoclonal trail antibodies against the TNF-related apoptosis, such as Apomab (TRAIL-receptor agonist), are also being explored and now are entering the clinical trial arena.
Non-surgical: The role of chemotherapy remains unclear. A poor 5-year survival and no difference in overall survival between patients managed with surgery alone (11.8%) and those managed with a combination of surgery and chemotherapy (4%) has been reported. Others recommended immediate surgical removal of the lesions and postoperative chemotherapy if possible to prevent metastatic spread of the disease. Given the poor prognosis of patients with dedifferentiated chondrosarcoma, National Comprehensive Cancer Network (NCCN) guidelines suggest treating dedifferentiated chondrosarcoma in a fashion similar to osteosarcoma. Radiation therapy can be considered (1) after incomplete resection, aiming at maximal local control (curative), (2) if resection is not feasible or would cause major morbidity (palliative).
Targeted treatments: A phase II trial investigates the use of perifosine, a modulator of membrane permeability, in patients with chemotherapy insensitive tumors including chondrosarcomas. Novel anti-folates, such as pemetrexed, are currently under active investigation in patients with chondrosarcoma, as is the combination of gemcitabine and docetaxel. Finally, small-molecule inhibitors, such as dasatinib, and monoclonal trail antibodies against the TNF-related apoptosis, such as Apomab (TRAIL-receptor agonist), are also being explored and now are entering the clinical trial arena.
Prognosis
The average time from diagnosis to the onset of metastatic disease is usually short. The anatomical site of metastases is the lungs (70-82%), the viscera (20%) and the skeleton (10%). Histologically, metastases consist only of the high-grade anaplastic component. There is no uniform guideline for the treatment of metastases.
The prognostic factors for patients with dedifferentiated chondrosarcomas are vague; metastatic disease at diagnosis, malignant fibrous histiocytoma dedifferentiation, and a high percentage of dedifferentiated component were related to poorer outcomes. Early diagnosis at a localized stage of disease through a careful biopsy and adequate surgical treatment may improve the survival of these patients. Metastatic disease at presentation is a strong negative predictive factor of patient survival. Tumor location at the pelvis has been reported as an independent risk factor for metastases and death.
Local recurrence and the histology of the dedifferentiated component have also been noted to be independent risk factors for metastases and death. Malignant fibrous histiocytoma dedifferentiation had a significantly worse prognosis compared with patients who had an osteosarcoma dedifferentiation. The rate of local recurrence seems to depend on the margins of tumor resection; as expected, radical or wide resection is associated with lower local reccurrence rates compared to inadequate resection. However, local tumor control does not seem to be related to a better rate of survival.
The prognostic factors for patients with dedifferentiated chondrosarcomas are vague; metastatic disease at diagnosis, malignant fibrous histiocytoma dedifferentiation, and a high percentage of dedifferentiated component were related to poorer outcomes. Early diagnosis at a localized stage of disease through a careful biopsy and adequate surgical treatment may improve the survival of these patients. Metastatic disease at presentation is a strong negative predictive factor of patient survival. Tumor location at the pelvis has been reported as an independent risk factor for metastases and death.
Local recurrence and the histology of the dedifferentiated component have also been noted to be independent risk factors for metastases and death. Malignant fibrous histiocytoma dedifferentiation had a significantly worse prognosis compared with patients who had an osteosarcoma dedifferentiation. The rate of local recurrence seems to depend on the margins of tumor resection; as expected, radical or wide resection is associated with lower local reccurrence rates compared to inadequate resection. However, local tumor control does not seem to be related to a better rate of survival.
Cytogenetics
Cytogenetics molecular
Dedifferentiated chondrosarcoma has a strong tumorigenicity and shows chondroblastic and osteoblastic characteristics in vitro and in vivo. The expression of PPAR-γ might have contributed to the multifunctional property of the cell line. This cell line showed extremely complicated karyotype based on cytogenetic analysis. Although no specific chromosomal abnormality has yet been identified; a part of the chromosome commonly demonstrated a repeated numerical aberration of +7, +8, +20, and +21. In addition, this cell line shared a part of cytogenetic findings with chondrosarcoma and osteosarcoma.
Genetics
Note
Controversy remains as to whether the anaplastic and cartilaginous components are derived from a common precursor cell, or whether they represent separate genotypic lineages (collision tumour). Molecular, genetic and epigenetic studies show that both tumor components share some genetic alterations; two clones derive from a single precursor but a substantial number of genetic alterations occur after the diversion of the two components, indicating that these two clones are separated in the early phases of the disease progress and further alterations are responsible for the switch to a high-grade anaplastic sarcoma.
Genes Involved and Proteins
Note
Tumor suppressor gene mutations may play a major role in the development, progression, and /or differentiation of tumors.
P53 gene: Mutations of p53 occur frequently in the oncogenesis of various mesenchymal neoplasms. Some authors reported that p53 overexpression was consistently present in dedifferentiated components with accompanied increased proliferative activity and an absence in low-grade cartilaginous component. It has been documented that the overexpression of p53 measured immunohistochemically is usually due to the accumulation of the mutated gene product, which exhibits a longer half-life than the wild-type protein. Recent genetic analyses revealed that p53 mutations were detected exclusively in dedifferentiated components.
Ras-genes: Activating mutations in ras genes (K-ras, H-ras, and N-ras) usually at codons 12, 13 and 61 are a common genetic abnormalities in human malignancies. Among the patients with dedifferentiated chondrosarcomas, those with H-ras mutation tended to have a worse prognosis than those without. Therefore, H-ras mutation may occur during the course of dedifferentiation and may also have some effect on malignant potential.
P53 gene: Mutations of p53 occur frequently in the oncogenesis of various mesenchymal neoplasms. Some authors reported that p53 overexpression was consistently present in dedifferentiated components with accompanied increased proliferative activity and an absence in low-grade cartilaginous component. It has been documented that the overexpression of p53 measured immunohistochemically is usually due to the accumulation of the mutated gene product, which exhibits a longer half-life than the wild-type protein. Recent genetic analyses revealed that p53 mutations were detected exclusively in dedifferentiated components.
Ras-genes: Activating mutations in ras genes (K-ras, H-ras, and N-ras) usually at codons 12, 13 and 61 are a common genetic abnormalities in human malignancies. Among the patients with dedifferentiated chondrosarcomas, those with H-ras mutation tended to have a worse prognosis than those without. Therefore, H-ras mutation may occur during the course of dedifferentiation and may also have some effect on malignant potential.
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 10629543 | 1999 | Molecular genetic characterization of both components of a dedifferentiated chondrosarcoma, with implications for its histogenesis. | Bovée JV et al |
| 3335575 | 1988 | Dedifferentiated chondrosarcoma. | Capanna R et al |
| 5566365 | 1971 | Dedifferentiation of low-grade chondrosarcomas. | Dahlin DC et al |
| 15523011 | 2004 | Dedifferentiated chondrosarcoma: the role of chemotherapy with updated outcomes. | Dickey ID et al |
| 3021775 | 1986 | Dedifferentiated chondrosarcoma. A report of the clinicopathological features and treatment of seventy-eight cases. | Frassica FJ et al |
| 17653762 | 2007 | Establishment of novel human dedifferentiated chondrosarcoma cell line with osteoblastic differentiation. | Kudo N et al |
| 22385450 | 2012 | Chondrosarcomas revisited. | Mavrogenis AF et al |
| 7481896 | 1995 | Dedifferentiated chondrosarcoma. | Mercuri M et al |
| 11172900 | 2001 | Chromosomal changes in a dedifferentiated chondrosarcoma: a case report and review of the literature. | O'Malley DP et al |
| 16826117 | 2006 | Survivorship analysis in patients with periosteal chondrosarcoma. | Papagelopoulos PJ et al |
| 12924447 | 2003 | Genetic and epigenetic alterations in tumor progression in a dedifferentiated chondrosarcoma. | Röpke M et al |
| 11301351 | 2001 | H-ras oncogene mutation in dedifferentiated chondrosarcoma: polymerase chain reaction-restriction fragment length polymorphism analysis. | Sakamoto A et al |
| 17653766 | 2008 | Dedifferentiated chondrosarcoma: our clinico-pathological experience and dilemmas in 25 cases. | Sopta J et al |
| 17473135 | 2007 | Dedifferentiated chondrosarcomas arising in preexisting osteochondromas. | Staals EL et al |
Citation
Andreas F Mavrogenis ; Panayiotis J Papagelopoulos
Bone: Dedifferentiated chondrosarcoma
Atlas Genet Cytogenet Oncol Haematol. 2012-03-01
Online version: http://atlasgeneticsoncology.org/solid-tumor/5337/bone-dedifferentiated-chondrosarcoma
