Alpha heavy chain disease
2016-06-01 Kenneth C. Anderson , Giada Bianchi Affiliation1.LeBow Institute for Myeloma Therapeutics and Jerome Lipper Multiple Myeloma Center, Department of Medical Oncology, Dana Farber Cancer Institute, Harvard Medical School, Boston, MA, 02115. [email protected]; [email protected]
Abstract
Alpha heavy chain disease (HCD) is the most prevalent form of heavy chain diseases, a rare family of syndromes associated with or representing a B cell malignancy variant. The hallmark characteristic and the pathogenic mechanism of HCD is the synthesis of a mutant, misfolded immunoglobulin heavy chain (IgH) which cannot form a quaternary conformation with the immunoglobulin light chain (IgL) and/or be degraded by the proteasome. The isotype of mutated IgH (α,γ or μ) determines the nomenclature of HCD subtypes. More than 400 cases of alpha HCD have been reported in the literature. The distinct epidemiology of the disease, affecting low socio-economical status individuals in the Mediterranean, North Africa, and Middle East, suggests an environmental etiologic agent. It typically affects individuals in their second and third decade of life, with a slight male predominance. Alpha HCD typically involves the small intestine (predominantly duodenum and jejunum), and presents as a malabsorption syndrome with symptoms and signs related to the severity and duration of involvement. A lymphomatous variant with predominant involvement of lymph nodes, spleen, and liver; as well as a respiratory variant with diffuse pulmonary infiltrates and restrictive pattern of respiratory function, have been reported. Diagnosis is based on laboratory findings and histologic analysis of involved organs. Based on the probable infectious pathogenesis, emphasis is on primary prevention via improvement of sanitary conditions and hygiene. Left untreated, alpha HCD locally progresses and eventually spreads systemically. A prolonged trial (> 6 months) of antimicrobial therapy is the first therapeutic approach even in the absence of a documented pathogen, followed by abdominal radiation and/or doxorubicin-based combination chemotherapy regimens plus minus surgical debulking. The five year overall survival rate after combination chemotherapy is 67%. Autologous hematopoietic stem cell transplantation should be considered in patients with relapsed/refractory disease.
Clinics and Pathology
Disease
Phenotype stem cell origin
Etiology
Epidemiology
Clinics
Pathology
Cytogenetics
Genes
Treatment
Evolution
Prognosis
Note
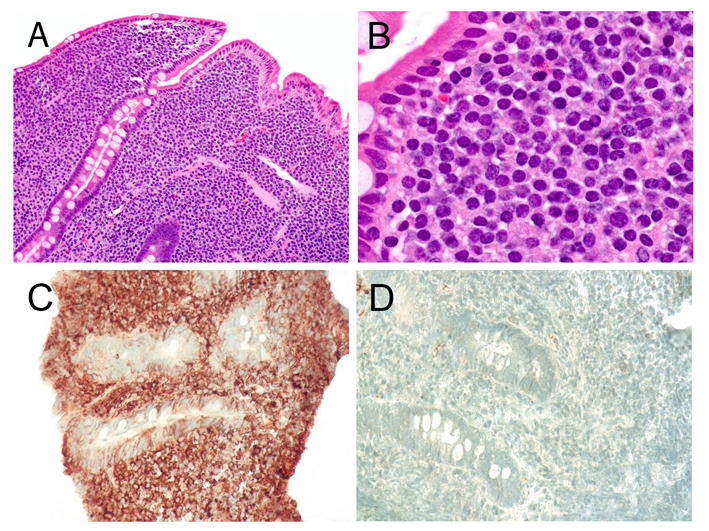
The abnormal Ig alpha heavy chain can manifest as hypogammaglobulinemia or a normal serum protein electrophoresis (SPEP). A broad monoclonal band migrating in the α 2- β region may be present and identified via immunofixation with anti IgA serum. The lymphoma variant associated with alpha HCD resembles mucosa-associated lymphoid tissue (MALT), and immunoproliferative small intestine disease (IPSID) has been diagnosed in this context. Pathologic analysis of IPDIS reveals a dense lymphoplasmacytic infiltrate of plasma cells admixed with small B lymphocytes separating the crypts and causing villous atrophy. Lymphoplasmacytic cells are monoclonal for cytoplasmic alpha chain in the absence of a light chain; plasma cells are CD138+ and CD20 negative; while small B lymphocytes express pan B-cell markers and lack CD5 and CD10.
Genes Involved and Proteins
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 9210703 | 1997 | Five-year results of the treatment of 23 patients with immunoproliferative small intestinal disease: a Turkish experience. | Akbulut H et al |
| 15542584 | 2005 | Immunoproliferative small intestinal disease (IPSID): a model for mature B-cell neoplasms. | Al-Saleem T et al |
| 829415 | 1976 | Alpha-chain disease and related small-intestinal lymphoma: a memorandum. | |
| 2920354 | 1989 | Treatment of alpha chain disease. Results of a prospective study in 21 Tunisian patients by the Tunisian-French intestinal Lymphoma Study Group. | Ben-Ayed F et al |
| 24683718 | 2014 | The heavy chain diseases: clinical and pathologic features. | Bianchi G et al |
| 4119805 | 1972 | Five cases of alpha chain disease. | Doe WF et al |
| 10626151 | 1999 | Heavy-chain diseases. | Fermand JP et al |
| 10235185 | 1999 | Alpha-heavy chain disease, Mediterranean lymphoma, and immunoproliferative small intestinal disease: a review of clinicopathological features, pathogenesis, and differential diagnosis. | Fine KD et al |
| 9482908 | 1998 | Frequent occurrence of deletions and duplications during somatic hypermutation: implications for oncogene translocations and heavy chain disease. | Goossens T et al |
| 3756829 | 1986 | Diagnostic value of upper intestinal fiber endoscopy in primary small intestinal lymphoma. A prospective study by the Tunisian-French Intestinal Lymphoma Group. | Halphen M et al |
| 2512818 | 1989 | Immunoproliferative small-intestinal disease. An immunohistochemical study. | Isaacson PG et al |
| 14724303 | 2004 | Immunoproliferative small intestinal disease associated with Campylobacter jejuni. | Lecuit M et al |
| 8313111 | 1994 | Immunoproliferative small intestinal disease: Mediterranean lymphoma and alpha heavy chain disease. | Martin IG et al |
| 18434654 | 2008 | Case records of the Massachusetts General Hospital. Case 13-2008. A 46-year-old man with rheumatoid arthritis and lymphadenopathy. | Munshi NC et al |
| 14724298 | 2004 | Bacterial infection and MALT lymphoma. | Parsonnet J et al |
| 15084705 | 2004 | Immunoproliferative small intestinal disease associated with Campylobacter jejuni. | Peterson MC et al |
| 16259867 | 2005 | Immunoproliferative small intestinal disease: current concepts. | Salem PA et al |
| 810152 | 1975 | Alpha chain disease: immunoglobulin abnormalities, pathogenesis and current concepts. | Seligmann M et al |
| 4177362 | 1968 | Alpha-chain disease: a new immunoglobulin abnormality. | Seligmann M et al |
| 4111693 | 1971 | Alpha-chain disease with involvement of the respiratory tract in a Dutch child. | Stoop JW et al |
| 3222174 | 1988 | A new form of alpha-chain disease with generalized lymph node involvement. | Takahashi K et al |
| 16026747 | 2005 | Heavy chain diseases. | Wahner-Roedler DL et al |
Summary
Note
Citation
Kenneth C. Anderson ; Giada Bianchi
Alpha heavy chain disease
Atlas Genet Cytogenet Oncol Haematol. 2016-06-01
Online version: http://atlasgeneticsoncology.org/haematological/2029/alpha-heavy-chain-disease
