i(9q) in ALL
2006-05-01 Patrick Koty , David H. Buss , Mark J. Pettenati , Noel A. Brownlee Affiliation1.Department of Pathology, Wake Forest University School of Medicine, Winston-Salem, NC 27157, USA
Clinics and Pathology
Disease
Precursor B-cell lymphoblastic leukemia
Phenotype stem cell origin
The cell of origin is thought to be a precursor B-lymphoblast. These cells are positive for terminal deoxynucleotidyl transferase, CD19, cytoplasmic CD79a, CD10, CD24. Variable expression for CD20 and CD22 may be seen. The myeloid lineage markers CD13 and CD33 may also be expressed
Etiology
Isochromosomes are relatively unusual and include i(6p), i(7q), i(9q), and i(17q).
Epidemiology
Precursor B-cell lymphoblastic leukemia is primarily a disease of children with most cases occurring before the age of six. Approximately 3000 new cases of lymphoblastic leukemia were reported in the United States in 2000.
The presence of isochromosomes is a relatively unusual finding. In the few published studies available, isochromosomes occur in between 1-4% of call cases of lymphoblastic leukemia, and were most commonly associated with a precursor B-cell immunophenotype. The most commonly seen isochromosome is i(9q), followed closely by i(17q), and i(7q).
The presence of isochromosomes is a relatively unusual finding. In the few published studies available, isochromosomes occur in between 1-4% of call cases of lymphoblastic leukemia, and were most commonly associated with a precursor B-cell immunophenotype. The most commonly seen isochromosome is i(9q), followed closely by i(17q), and i(7q).
Clinics
The presenting features of lymphoblastic leukemia include evidence of bone marrow failure including anemia, thrombocytopenia, and leukopenia. The leukocyte count may be elevated, normal, or even decreased. Other signs and symptoms may include hepatosplenomegaly, lymphadenopathy, bone pain, and arthralgias. A small number of patients may present with lymphoblastic lymphoma.
Isochromosome 9q is generally associated with patient age greater than 10 years and a pre-B cell immunophenotype. In a series of 28 patients with i(9q), patients ranged in age from 1 to 17 years (median age 8 years).
Isochromosome 9q is generally associated with patient age greater than 10 years and a pre-B cell immunophenotype. In a series of 28 patients with i(9q), patients ranged in age from 1 to 17 years (median age 8 years).
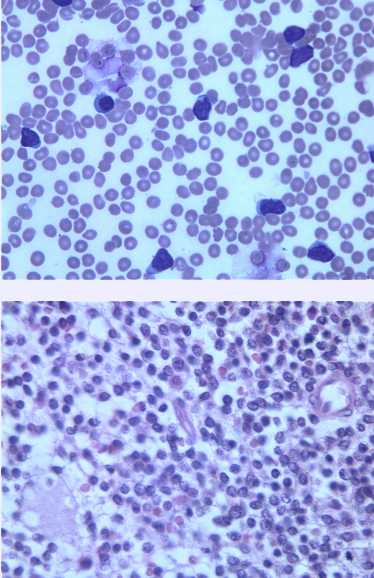
Top: Peripheral blood smear stained with Wrights Giemsa stain obtained from a patient harboring an isochromosome 9q demonstrating a lymphocytosis. Numerous lymphoblasts characterized by high nuclear-cytoplasmic ratios, an open chromatin pattern, and nucleoli are present. This smear also demonstrates profound thrombocytopenia and neutropenia.
Bottom Bone marrow biopsy section obtained from a patient with precursor B-cell lymphoblastic leukemia harboring an isochromosome 9q. Lymphoblasts have largely replaced the marrow space usually occupied with numerous myeloid and erythroid precursors.
Cytology
Precursor B-cell lymphoblastic leukemia is a neoplasm composed of small to medium-sized blast cells with high nuclear to cytoplasmic ratios, moderately condensed to open chromatin pattern, and inconspicuous nucleoli
Pathology
The cells of lymphoblastic lymphoma may demonstrate a range of sizes. They may vary from small round cells with high nuclear-cytoplasmic ratios to larger cells with more cytoplasm (usually blue to grey-blue cytoplasm). Nuclear chromatin is usually uncondensed. Nucleoli are generally inconspicuous.
Treatment
Treatment is divided in induction, consolidation, and maintenance chemotherapy. Three drug induction chemotherapy including vincristine, a steroid (e.g. dexamethasone), and L-asparaginase in conjunction with intrathecal therapy induces a complete remission rate greater than 95%. Daunorubicin may be added for high risk patients. Consolidation therapy may involve high-dose methotrexate, the same drugs used in induction, or other drug combinations. Maintenance therapy in most protocols typically involves the use of oral methotrexate (weekly) and daily oral mercaptopurine.
Evolution
Precursor B-cell lymphoblastic leukemia progresses quickly if left untreated; however, this disease is one of the most curable cancers with survival rates now at its all-time peak. Older and very young patients tend to have lower survival rates
Prognosis
The prognosis of B-cell lymphoblastic leukemia is excellent. The overall complete remission rate is approximately 95% in pediatric patients and around 70-75% for adults.
Cytogenetics
Note
Several isochromosome anomalies are readily identified in childhood ALL. These include: formation of chromosomes i(6p), i(7q), i(9q), and i(17q). The i(9q) can be found as a sole anomaly or in combination with a number of different chromosome anomalies.
Cytogenetics morphological
The i(9q) can be fairly well recognized with two copies of the long arm of chromosome 9 accompanied with the loss of the short arm of chromosome 9p thus resulting in an unbalanced anomaly loss of 9p and gain of 9q.
Additional anomalies
isochromosome 9q was found associated with other non-random chromosomal abnormalities including t(1;19)(q23;p13) (involving the PBX and E2A genes), a finding in 4 of 28 cases, and t(9;22)(q34;q11) (involving fusion of the BCR and ABL genes) in one case. In a series of ten Down syndrome patients, i(9q) was identified in 3 of 10 cases.
Genes Involved and Proteins
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 11187913 | 2000 | Children's Cancer Group trials in childhood acute lymphoblastic leukemia: 1983-1995. | Gaynon PS et al |
| 2149960 | 1990 | Clinical and biological characteristics of acute lymphocytic leukemia in children with Down syndrome. | Kalwinsky DK et al |
| 8889503 | 1996 | Isochromosomes in acute lymphoblastic leukaemia: i(21q) is a significant finding. | Martineau M et al |
| 1571550 | 1992 | Isochromosomes in childhood acute lymphoblastic leukemia: a collaborative study of 83 cases. | Pui CH et al |
| 11187912 | 2000 | Long-term results of four consecutive trials in childhood ALL performed by the ALL-BFM study group from 1981 to 1995. Berlin-Frankfurt-Münster. | Schrappe M et al |
| 2918757 | 1989 | Isochromosome 9q in acute lymphoblastic leukemia: a new non-random finding. | Shippey CA et al |
Summary
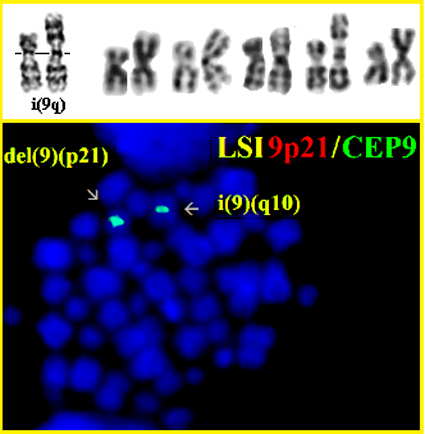
i(9q) iso (9q) G- banding - Courtesy of Andrew Carroll (Left); - Courtesy Adriana Zamecnikova (five rtight). Fluorescence in situ hybridization with LSI CDKN2A/CEP9 probe (Vysis/Abbott molecular, US) showing deletion of CDKN2A located on 9p (red signal) as a result of isochromosome formation (A) and deletion of both genes as a result of simultaneous 9p deletion and isochromosome formation (B).
Citation
Patrick Koty ; David H. Buss ; Mark J. Pettenati ; Noel A. Brownlee
i(9q) in ALL
Atlas Genet Cytogenet Oncol Haematol. 2006-05-01
Online version: http://atlasgeneticsoncology.org/haematological/1066/i(9q)-in-all
