Acute myeloid leukemia with myelodysplasia related changes
2017-01-01 Andreas Neubauer , Alexandra Nagy Affiliation1.Howard Hughes Medical Institute and the Department Pathology, Beckman Center for Molecular and Genetic Medicine, Stanford University, Stanford, California 94305, USA; [email protected] (A Na); Dept. Internal Medicine and Hematology, Oncology and Immunology, Philipps University Marburg,Germany; [email protected] (A Ne)
Abstract
Acute myeloid leukemia (AML) is a heterogeneous clonal disorder with two prominent features: i) hematopoietic progenitor cells loose the ability to differentiate normally and ii) the transformed leukemia cells show an impaired regulation of myeloid proliferation.
Clinics and Pathology
Disease
Etiology
Epidemiology
Cytology
Other features
Treatment
Prognosis
Cytogenetics
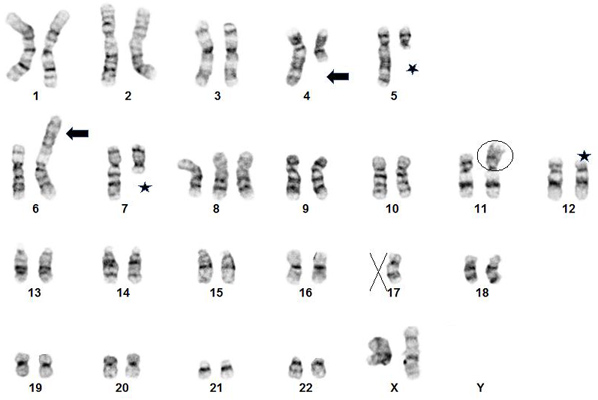
Genes Involved and Proteins
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 27069254 | 2016 | The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. | Arber DA et al |
| 12760285 | 2003 | Prognostic impact of acute myeloid leukemia classification. Importance of detection of recurring cytogenetic abnormalities and multilineage dysplasia on survival. | Arber DA et al |
| 24695467 | 2014 | Granulocyte, monocyte and blast immunophenotype abnormalities in acute myeloid leukemia with myelodysplasia-related changes. | Ayar SP et al |
| 26078355 | 2015 | Next-generation sequencing of FLT3 internal tandem duplications for minimal residual disease monitoring in acute myeloid leukemia. | Bibault JE et al |
| 23634996 | 2013 | Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. | Ley TJ et al |
| 24136165 | 2013 | The genetic basis of myelodysplasia and its clinical relevance. | Cazzola M et al |
| 23690127 | 2013 | Pediatric acute myeloid leukemia as classified using 2008 WHO criteria: a single-center experience. | Davis KL et al |
| 17019734 | 2006 | Acute myeloid leukemia: epidemiology and etiology. | Deschler B et al |
| 17126723 | 2006 | Acute myeloid leukaemia. | Estey E et al |
| 20203266 | 2010 | Multilineage dysplasia has no impact on biologic, clinicopathologic, and prognostic features of AML with mutated nucleophosmin (NPM1). | Falini B et al |
| 16417922 | 2006 | Evaluation of CD7 and terminal deoxynucleotidyl transferase (TdT) expression in CD34+ myeloblasts from patients with myelodysplastic syndrome. | Font P et al |
| 19429869 | 2009 | AML with mutated NPM1 carrying a normal or aberrant karyotype show overlapping biologic, pathologic, immunophenotypic, and prognostic features. | Haferlach C et al |
| 23906712 | 2013 | Structural and functional properties of platelet-derived growth factor and stem cell factor receptors. | Heldin CH et al |
| 26084204 | 2016 | Allogeneic hematopoietic stem cell transplant overcomes poor prognosis of acute myeloid leukemia with myelodysplasia-related changes. | Ikegawa S et al |
| 21779483 | 2011 | Genetic abnormalities and challenges in the treatment of acute myeloid leukemia. | Kumar CC et al |
| 20471513 | 2010 | Detection of t(3;5) and NPM1/MLF1 rearrangement in an elderly patient with acute myeloid leukemia: clinical and laboratory study with review of the literature. | Lim G et al |
| 24970933 | 2014 | Driver somatic mutations identify distinct disease entities within myeloid neoplasms with myelodysplasia. | Malcovati L et al |
| 20581309 | 2010 | Multilineage dysplasia (MLD) in acute myeloid leukemia (AML) correlates with MDS-related cytogenetic abnormalities and a prior history of MDS or MDS/MPN but has no independent prognostic relevance: a comparison of 408 cases classified as "AML not otherwise specified" (AML-NOS) or "AML with myelodysplasia-related changes" (AML-MRC). | Miesner M et al |
| 19277035 | 2009 | Heterogeneity within AML with CEBPA mutations; only CEBPA double mutations, but not single CEBPA mutations are associated with favourable prognosis. | Pabst T et al |
| 21917154 | 2011 | Current findings for recurring mutations in acute myeloid leukemia. | Takahashi S et al |
| 22552007 | 2012 | EuroFlow antibody panels for standardized n-dimensional flow cytometric immunophenotyping of normal, reactive and malignant leukocytes. | van Dongen JJ et al |
| 26071460 | 2015 | Acute Myeloid Leukemia With Myelodysplasia-Related Changes. | Vardiman J et al |
| 27387988 | 2017 | Assessment of myeloid and monocytic dysplasia by flow cytometry in de novo AML helps define an AML with myelodysplasia-related changes category. | Weinberg OK et al |
| 19131546 | 2009 | Clinical characterization of acute myeloid leukemia with myelodysplasia-related changes as defined by the 2008 WHO classification system. | Weinberg OK et al |
| 23737874 | 2013 | Characteristics of the four subtypes of myelodysplastic/myeloproliferative neoplasms. | Wu H et al |
| 24861848 | 2014 | Characteristics of acute myeloid leukemia with myelodysplasia-related changes: A retrospective analysis in a cohort of Chinese patients. | Xu XQ et al |
| 27496968 | 2017 | Acute leukaemia and myelodysplastic syndromes with chromosomal rearrangement involving 11q23 locus, but not MLL gene. | Zuo W et al |
Citation
Andreas Neubauer ; Alexandra Nagy
Acute myeloid leukemia with myelodysplasia related changes
Atlas Genet Cytogenet Oncol Haematol. 2017-01-01
Online version: http://atlasgeneticsoncology.org/haematological/2041/acute-myeloid-leukemia-with-myelodysplasia-related-changes
