CASR (Calcium-Sensing Receptor)
2013-09-01 Bryan Ward , Aaron Magno , Thomas Ratajczak AffiliationDepartment of Endocrinology, Diabetes, Sir Charles Gairdner Hospital, UWA Centre for Medical Research, The University of Western Australia, Nedlands, Western Australia, 6009, Australia
Identity
HGNC
LOCATION
3q21.1
LOCUSID
ALIAS
CAR,EIG8,FHH,FIH,GPRC2A,HHC,HHC1,HYPOC1,NSHPT,PCAR1,hCasR
FUSION GENES
DNA/RNA
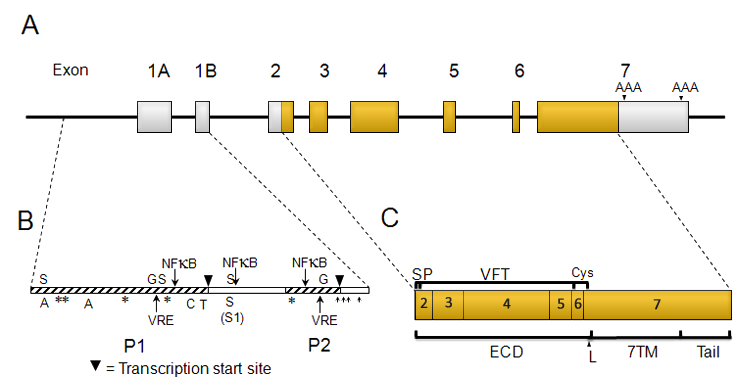
Figure 1. Schematic representation of the calcium-sensing receptor (CaSR) gene structure (A), promoter location and features (B) and protein structural arrangement (C). The CaSR mRNA is transcribed from part of exon 2, all of exons 3 to 6 and part of exon 7. Exons that comprise the CaSR protein are shaded yellow; untranslated exons are left unshaded. Note that intronic regions are not drawn to scale. The location of polyadenylation sites (AAA) within the untranslated region of exon 7 are arrowed. In B, the spatial relationship between promoters P1 and P2 (hatched) and untranslated exons 1A and 1B (unshaded) is highlighted along with the position of various transcription factor binding sites and regulatory elements: C, CCAAT box; T, TATA box; A, Ap-1 sites; *, serum response elements; VRE, vitamin D response elements; G, glial cells missing-2 response element; ↑, Sp1 sites; NFκB, NFκB response elements; S, STAT sites (S1 regulates IL-6 response). The CaSR protein (C) is composed of the extracellular domain (ECD) consisting of a signal peptide (SP), Venus Fly Trap (VFT) domain and cysteine-rich domain (Cys) connected by a small linker region (L) to the seven transmembrane domain (7TM) and intracellular tail, both encoded by exon 7.
Description
The human CaSR gene maps to 3q13.3-21, is approximately 103 kb in length and contains 8 exons (exons 1A and 1B and exons 2-7) (Garrett et al., 1995; Janicic et al., 1995; Hendy et al., 2009). The full length CaSR protein is translated from part of exon 2, all of exons 3-6 and part of exon 7 (Figure 1). Exons 1A and 1B are not translated. An alternatively spliced, functional variant of the receptor lacking exon 5 has been reported (Rodriguez et al., 2005a). The CaSR gene has two promoters, an upstream promoter (P1) containing a TATA box and CCAAT box and an additional promoter (P2) with Sp1 sites that cluster near the transcriptional start site (Figure 1; Chikatsu et al., 2000; Canaff et al., 2008; Hendy et al., 2009). The two promoters yield alternative transcripts containing either exon 1A or exon 1B spliced to exon 2 (Chikatsu et al., 2008; Hendy et al., 2009). Both promoters contain vitamin D response elements as well as response motifs for NF-κB and glial cells missing-2 (Canaff and Hendy, 2002; Canaff and Hendy, 2005; Canaff et al., 2009). The upstream promoter region contains Stat1/stat3 elements which allow for response to interleukin-6 (Canaff et al., 2008). Use of differential polyadenylation signals in exon 7 appear to lead to at least two different-sized 3 untranslated regions (Figure 1; Garrett et al., 1995).
Proteins
Note
The full length human CaSR mRNA encodes a protein of 1078 amino acids consisting of a 612 amino acid signal peptide/extracellular domain (ECD), a 250 amino acid seven transmembrane domain (7TM) and an unusually long 216 amino acid intracellular tail (Garrett et al., 1995; Hu and Spiegel, 2003) (Figure 1). The NH2-terminal signal peptide is 19 amino acids in length and directs the nascent protein to the endoplasmic reticulum (ER) where it is subsequently removed (Hu and Spiegel, 2003; Pidasheva et al., 2005; Hendy et al., 2009). The ECD is composed of a bilobed Venus flytrap (VFT) domain followed by a cysteine-rich domain connected via a peptide linker region to the 7TM which in addition to the membrane α-helices also contains three intra- and three extra-cellular loops; the final TM α-helix is connected to the intracellular tail, the membrane proximal domain of which is important for receptor cell expression and intracellular signalling (Ray et al., 1997; Hu and Spiegel, 2003). The CaSR protein is processed as a dimer in the ER via covalent intermolecular disulphide bonds and hydrophobic interactions and functions as a dimer when mature (Bai et al., 1998; Bai et al., 1999; Zhang et al., 2001; Pidasheva et al., 2006). Essentially, agonist binding to a cleft between the VFT lobes of each monomer leads to their closure and rotation about the VFT dimer interface thus transmitting a conformational change to the cysteine-rich domain which in turn allows movement of the 7TM α-helices with respect to one another resulting in connection of G proteins to the intracellular loops and initiation of signalling pathways (Hu and Spiegel, 2003). The CaSR contains 11 potential N- linked glycosylated sites in the ECD and is glycosylated in the ER with high mannose carbohydrates (immature receptor) after which it is transported to the Golgi where it is further modulated with complex carbohydrates (mature receptor) (Ray et al., 1998). Western blot analysis of protein extracted from cells containing mature and immature CaSR reveal bands at 150 kDa and 130 kDa, respectively. The CaSR contains five potential sites for protein kinase C phosphorylation, two in intracellular loops 1 and 3 and three in the intracellular tail and two potential sites for protein kinase A phosphorylation in the intracellular tail (Garrett et al., 1995; Bosel et al., 2003).
Description
The CaSR was first cloned from bovine parathyroid cells by Brown and coworkers in 1993 and the human receptor was cloned from an adenomatous parathyroid gland in 1995 (Brown et al., 1993; Garrett et al., 1995). The CaSR is a G protein-coupled receptor belonging to Group II of Family C, G protein-coupled receptors and conforms to a typical G protein-coupled receptor structure with a large extracellular domain, a seven transmembrane spanning domain and a rather large intracellular tail (Brown and MacLeod, 2001; Hu and Spiegel, 2003). The CaSR is promiscuous, activating a variety of signalling pathways via a host of ligands (in addition to Ca2+) in a cell/tissue type-specific manner (Brown and MacLeod, 2001; Magno et al., 2011b). The receptors primary function is in the maintenance of calcium homeostasis in the body, but other functions have more recently come to light (see below).
Expression
The CaSR has a widespread tissue distribution in the body including those tissues which are important in the maintenance of calcium homeostasis, namely the chief cells of the parathyroid gland where it is responsible for regulating parathyroid hormone (PTH) secretion, the C cells of the thyroid whereby it controls calcitonin secretion, the kidney where it controls calcium reabsorption, the placenta whereby it controls calcium transport from mother to foetus and in cartilage and bone cells, (chondrocytes, osteoblasts and osteoclasts) in which it has important effects on the laying down and maintenance of the skeleton (Magno et al., 2011b; Riccardi and Kemp, 2012). The CaSR is also expressed in intestinal epithelial cells where it serves to regulate intestinal uptake of calcium by directly modulating responsiveness to 1,25-dihydroxyvitamin D (Egbuna et al., 2009). Apart from tissues which regulate calcium homeostasis, the CaSR is also expressed in many tissues outside this realm including the breast, ovary, uterus, testis, prostate and germ cells, the tongue, oesophagus, stomach and pancreas as well as the heart, various parts of the brain (including the subfornical organ and olfactory bulbs, hippocampus, hypothalamus and cerebellum), pituitary, lens epithelium and skin (Brown and MacLeod, 2001; Magno et al., 2011b; Riccardi and Kemp, 2012). The function of the CaSR in many of these tissues is still largely unknown.
Localisation
As expected for a G protein-coupled receptor, the CaSR localizes to the plasma membrane of the cells in which it is expressed. However, there is accumulating evidence for a large intracellular pool of receptor that localizes to the ER/Golgi awaiting agonist driven trafficking to the plasma membrane, a mechanism thought to regulate membrane CaSR abundance in the chronic presence of agonist (Grant et al., 2011). While the CaSR does undergo endocytosis and is targeted to the lysosome, it does not undergo substantial desensitization and recycling as occurs with many other G protein-coupled receptors (Grant et al., 2011). In the chief cells of the parathyroid gland, CaSR is located in caveolae, flask-like invaginations of the plasma membrane that contain various signalling molecules and scaffolding proteins such as filamin-A and caveolin-1 to which the CaSR is anchored (Kifor et al., 1998). In various parts of the kidney tubule (proximal tubule, cortical thick ascending limb, distal convoluted tubule, medullary collecting duct) the membrane bound CaSR may be located apically or basolaterally or both depending on its specific function(s) in these compartments (Riccardi and Kemp, 2012). For example, the apically located CaSR in the medullary collecting duct inhibits insertion of AQP2 water channels and promotes activation of the B1 subunit of the vacuolar H+-ATPase in the apical membrane, thus delivering a less concentrated and more acidified urine (Sands et al., 1998; Procino et al., 2004; Riccardi and Kemp, 2012). Likewise in the gastrointestinal tract, the CaSR is expressed both on the apical and basolateral membranes of the gastrin secreting G cells of the stomach indicating that it can sense and respond to nutrient levels both in the lumen and in the blood, whereas CaSR in colonic epithelial cells, whether it is expressed apically or basolaterally, can mediate cAMP-mediated fluid secretion (Conigrave and Brown, 2006).
Function
The primary function of the CaSR is in the maintenance of calcium homeostasis through regulation of PTH secretion and reabsorption of calcium from the kidney tubules. PTH has effects on bone resorption, intestinal uptake of calcium (via production of 1,25-dihydroxyvitamin D) and calcium reabsorption from the kidney, all combining to restore calcium in the extracellular fluid to a concentration within the narrow range 1.1 - 1.3 mM Ca2+ (Tfelt-Hansen and Brown, 2005). However, the CaSR is now known to be a multifunctional receptor with important influences on major cellular processes that include not only entero-endocrine secretion but control of gene expression and cell differentiation, cellular proliferation, apoptosis, chemotaxis, cytoskeletal organization and the regulation of ion transport and the activity of ion channels (Tfelt-Hansen and Brown, 2005; Riccardi and Kemp, 2012). It achieves this enormous diversity of function by activating an array of cell signalling pathways in a tissue and ligand-dependent manner, with partner binding proteins also playing an important role (Brennan and Conigrave, 2009; Magno et al., 2011b). The CaSR can be activated not only by Ca2+ ions but by other di-, tri- and polyvalent cations including polyamines such as spermine, aminoglycoside antibiotics such as neomycin and polypeptides including amyloid β-peptide. Receptor activity is also modulated by pH and salinity and can be potentiated (in the presence of direct agonist) by allosteric activators such as L-amino acids and type II calcimimetics (Nemeth et al., 1998; Conigrave et al., 2000; Brown and MacLeod, 2001; Magno et al., 2011b). The receptor, upon activation, can couple to Gq/11, Gi/0, G12/13 and Gs G protein families to regulate a variety of signalling molecules including phosphatidylinositol-specific phospholipase C (PLC) (and hence PKC and release of intracellular Ca2+ from intracellular stores), as well as phospholipase A2, phosphatidylinositol 3-kinase (which in turn affects Akt signalling), phospholipase D and Rho and MAP kinases (including ERK1/ERK2) (Brennan and Conigrave, 2009; Magno et al., 2011b). When coupled to Gs and Gi the receptor can stimulate or inhibit cAMP production, respectively (Mamillapalli et al., 2008).
The precise pathway(s) involved in CaSR-mediated inhibition of PTH have yet to be completely elucidated, however the associated reduction in PTH mRNA levels involves an increase in intracellular Ca2+, suggesting a role for PLC activation (Ritter et al., 2008). The CaSR has several important homeostatic functions in the kidney depending on its location. In the proximal tubule, CaSR stimulation reverses the inhibitory effects of PTH on phosphate reabsorption via the phosphate transporters NaPi-IIa/NaPi-IIc and also blocks 2,5-hydoxyvitamin D3-1 α-hydroxylase. In the thick ascending limb of Henles loop, stimulation of basolaterally localized CaSR reduces potassium cycling (by decreasing the activity of the 70-pS channel) as well as NaCl transport and paracellular reabsorption of Mg2+ and Ca2+. In the distal convoluted tubule, the CaSR is located both apically and basolaterally, in the former it is linked to the receptor potential vanilloid member 5 (TPRV5) and stimulation of the CaSR therefore increases uptake of Ca2+ ions. Basolaterally, CaSR activation inhibits the activity of plasma membrane Ca2+-ATPase 1b and decreases expression of the K+ channel, Kir4.1 resulting in inhibition of basolateral K+ recycling. Activation of apically located CaSR in the medullary collecting duct reduces osmotic water permeability (creating less concentrated urine) by inhibiting vasopressin-induced insertion of AQP2 water channels and increases the activity of H+ -ATPase (making urine more acidic). These effects reduce the likelihood of kidney stone formation (see recent reviews that discuss the functional homeostatic role for the receptor in the kidney by Magno et al., 2011b and Riccardi and Kemp, 2012). The CaSR is also expressed in regions of the kidney that do not relate to Ca2+ or other mineral ion homeostasis. Activation of the CaSR expressed in the juxtaglomerular cells of the afferent arteriole of the kidney inhibits release of renin, thus exerting influence over the renin-angiotensin system that controls blood pressure (Atchison et al., 2010) while stimulation of the CaSR in the podocytes of the glomerular filter has been shown to effect the cytoskeletal integrity and viability of these cells suggesting an important role for the receptor in proper renal filtration (Oh et al., 2011).
The CaSR is expressed along the whole length of the gastrointestinal tract where it plays important roles in nutrient sensing, the regulation of fluid secretion, hormone release and cell differentiation/apoptosis (Conigrave and Brown, 2006; Geibel and Hebert, 2009). Recent data show that taste buds contain the CaSR and that agonists of the CaSR enhance taste perception while antagonists of the CaSR suppress it (Ohsu et al., 2010). The receptor is also expressed in the basal cells of the oesophagus where stimulation results in an increase in IL-8 secretion, the physiological importance of which is yet to be determined (Justinich et al., 2008). In the stomach, the CaSR plays a clear role in the regulation of gastrin and gastric acid release from G cells and parietal cells, respectively (Conigrave and Brown, 2006; Geibel and Hebert, 2009). In the duodenum, amino acid stimulation of the CaSR in I cells of the small intestine leads to release of cholecystokinin a hormone important for gall bladder contraction, pancreatic enzyme secretion and gastric emptying (Wang et al., 2011). CaSR expression in the acinar cells of the pancreas and in pancreatic duct cells suggests a role for the receptor in fluid secretion and/or the secretion of enzymes from the pancreas (Racz et al., 2002; Riccardi and Kemp, 2012). The proper regulation of fluid secretion from the pancreatic ducts by the CaSR is thought to be important in the prevention of pancreatic stones and pancreatitis (Riccardi and Kemp, 2012). In addition, activation of the CaSR expressed in the β-cells of the pancreatic islets of Langerhans can modulate insulin secretion and this has implications for the onset and progression of diabetes (Gray et al., 2006; Squires et al., 2000). CaSR expression in colonic epithelial cells is required for the transition of cells along the crypt from a proliferative to a differentiated state, thus the presence of receptor in these cells is thought to be important in preventing colon cancer (Whitfield, 2009). Agonist activation of the CaSR in the colon can suppress cAMP-mediated fluid loss and is important in the control of NaCl and water absorption (Geibel and Hebert, 2009). It has been proposed that calcimimetics could be used to prevent diarrhoea/fluid loss associated with bacterial toxins in diseases such as cholera (Geibel et al., 2006).
In the lactating breast, expression of the CaSR in mammary epithelial cells can regulate parathyroid hormone-related protein (PTHrP) production and adjust uptake of calcium into milk according to calcium availability (VanHouten et al., 2004). In the normal breast the CaSR has tumour suppressor properties acting in concert with the BRCA1 tumour suppressor to decrease levels of the antiapoptotic protein, survivin, and increase sensitivity to paclitaxel, a drug commonly used in breast cancer treatment (Promkan et al., 2011). However, if expressed in malignant breast cells, the receptor may actually aid bone metastasis (see below under hypercalcaemia of malignancy). With relevance to its apparent role in metastasis, the CaSR has been shown to couple to integrins thereby promoting tumour cell adhesion and migration (Tharmalingham et al., 2011). The CaSR can also bind the focal adhesion protein, testin, that is known to have important effects on cell spreading and motility (Magno et al., 2011a).
In the brain, The CaSR is highly expressed in the subfornical organ and potentiates neuronal, hyperpolarization-activated inward currents, consistent with the bursting of action potentials in these neurons that has also been shown to be CaSR-potentiated (Washburn et al., 2000; Yano et al., 2004). The expression of the CaSR in the subfornical organ, which is a thirst control centre, suggests that the receptor plays a crucial role in fluid and electrolyte homeostasis. The CaSR also controls neuronal excitability in a number of other parts of the brain by regulating ion channels and this may contribute to its apparent role in epilepsy (Kapoor et al., 2008; Riccardi and Kemp, 2012). For example, in the hippocampus, CaSR-mediated activation of a voltage-independent Na+ leak conductance channel leads to neuronal excitation (Lu et al., 2010). In the hippocampus, increasing expression of the CaSR during the first weeks of life correlate with long-term potentiation indicating that the CaSR may play a role in cognitive functions such as memory and learning (Brown and MacLeod, 2001; Yano et al., 2004). The CaSR has important regulatory effects on the developing nervous system, for example, activation of the CaSR appears to be critical for the expansion and differentiation of oligodendrocyte progenitor cells and the generation of myelin in preoligodendrocytes (Chattopadhyay et al., 2008). Stimulation of CaSR is required for the production of a cofactor, tetrahydrobiopterin, essential for the activation of nitrous oxide that is produced (in its inactive form) in response to amyloid β peptide-mediated activation of the receptor (Dal Pra et al., 2005). Hence, CaSR may play an important role in late onset Alzheimers disease that is characterized by nitrous oxide-mediated neuronal damage. In the pituitary gland, activation of the CaSR stimulates cAMP production via coupling to Gαs with subsequent secretion of PTHrP and ACTH (Mamillapalli and Wysolmerski, 2010).
The CaSR is expressed and plays a functionally important role in various bone cells including osteoblasts/osteocytes and osteoclasts and their precursors, bone marrow derived stromal cells, monocyte-macrophage cells, chondrocytes and haematopoietic stem cells (Yamaguchi, 2008). Targeted depletion of the CaSR induced in mouse embryonic chondrocytes and osteoblasts has revealed that the CaSR is absolutely required for growth plate and skeletal development (Chang et al., 2008). Activation of the CaSR in osteoblasts is required for osteoblast differentiation, proliferation and mineralization (Yamaguchi, 2008; Dvorak-Ewell et al., 2011). In addition, high Ca2+-induced apoptosis of osteoclasts is mediated through nuclear translocation of NF-κB which in turn is dependent on CaSR stimulation and activation of PLC (Mentaverri et al., 2006). The CaSR also appears to be important in osteoclastogenesis as shown in studies with bone marrow cells from CaSR knockout mice (Dvorak-Ewell et al., 2011). The CaSR is required for haemopoietic stem cells to lodge in the endosteal niche of the bone marrow - this has implications for the proper functioning of erythropoiesis (Adams et al., 2006). The CaSR appears to contribute, albeit indirectly, to the formation of teeth and the development of dental alveolar bone (Sun et al., 2010).
The CaSR also has established roles in other organs and tissues including the heart and circulatory system. In the heart, the receptor can augment angiotensin II-mediated cardiac hypertrophy in cardiomyocytes, while CaSR-mediated production of nitrous oxide can lead to vasodilation in human aortic epithelial cells with subsequent effects on blood pressure (Ziegelstein et al., 2006; Wang et al., 2008). The CaSR has also been shown to mediate the cardio-protective effects of ischaemic preconditioning (Sun and Murphy, 2010). Expression of the CaSR in vascular smooth muscle cells of human arteries appears to be important in preventing arterial calcification (Alam et al., 2009). The CaSR appears to play an important role in the differentiation of keratinocytes and their survival (Tu et al., 2008). Lens epithelial cells express CaSR mRNA and protein and stimulation of the receptor regulates a calcium-activated potassium channel - it is likely that the receptor contributes to lens integrity (Chattopadhyay et al., 1997; Brown and MacLeod, 2001).
The receptor also has functional effects on reproduction and development (Riccardi and Kemp, 2012). The CaSR is expressed in ovarian surface cells and ova (where it is important for development and maturation), sperm (where it is important for maturation, motility and fertilization) and uterus (where it plays roles in implantation and embryonic development). Hence its proper expression has important implications for fertility. In addition the receptor plays a critical role in the placenta and in embryonic and foetal development of organs such as the lung, brain and nervous system (Riccardi and Kemp, 2012).
The precise pathway(s) involved in CaSR-mediated inhibition of PTH have yet to be completely elucidated, however the associated reduction in PTH mRNA levels involves an increase in intracellular Ca2+, suggesting a role for PLC activation (Ritter et al., 2008). The CaSR has several important homeostatic functions in the kidney depending on its location. In the proximal tubule, CaSR stimulation reverses the inhibitory effects of PTH on phosphate reabsorption via the phosphate transporters NaPi-IIa/NaPi-IIc and also blocks 2,5-hydoxyvitamin D3-1 α-hydroxylase. In the thick ascending limb of Henles loop, stimulation of basolaterally localized CaSR reduces potassium cycling (by decreasing the activity of the 70-pS channel) as well as NaCl transport and paracellular reabsorption of Mg2+ and Ca2+. In the distal convoluted tubule, the CaSR is located both apically and basolaterally, in the former it is linked to the receptor potential vanilloid member 5 (TPRV5) and stimulation of the CaSR therefore increases uptake of Ca2+ ions. Basolaterally, CaSR activation inhibits the activity of plasma membrane Ca2+-ATPase 1b and decreases expression of the K+ channel, Kir4.1 resulting in inhibition of basolateral K+ recycling. Activation of apically located CaSR in the medullary collecting duct reduces osmotic water permeability (creating less concentrated urine) by inhibiting vasopressin-induced insertion of AQP2 water channels and increases the activity of H+ -ATPase (making urine more acidic). These effects reduce the likelihood of kidney stone formation (see recent reviews that discuss the functional homeostatic role for the receptor in the kidney by Magno et al., 2011b and Riccardi and Kemp, 2012). The CaSR is also expressed in regions of the kidney that do not relate to Ca2+ or other mineral ion homeostasis. Activation of the CaSR expressed in the juxtaglomerular cells of the afferent arteriole of the kidney inhibits release of renin, thus exerting influence over the renin-angiotensin system that controls blood pressure (Atchison et al., 2010) while stimulation of the CaSR in the podocytes of the glomerular filter has been shown to effect the cytoskeletal integrity and viability of these cells suggesting an important role for the receptor in proper renal filtration (Oh et al., 2011).
The CaSR is expressed along the whole length of the gastrointestinal tract where it plays important roles in nutrient sensing, the regulation of fluid secretion, hormone release and cell differentiation/apoptosis (Conigrave and Brown, 2006; Geibel and Hebert, 2009). Recent data show that taste buds contain the CaSR and that agonists of the CaSR enhance taste perception while antagonists of the CaSR suppress it (Ohsu et al., 2010). The receptor is also expressed in the basal cells of the oesophagus where stimulation results in an increase in IL-8 secretion, the physiological importance of which is yet to be determined (Justinich et al., 2008). In the stomach, the CaSR plays a clear role in the regulation of gastrin and gastric acid release from G cells and parietal cells, respectively (Conigrave and Brown, 2006; Geibel and Hebert, 2009). In the duodenum, amino acid stimulation of the CaSR in I cells of the small intestine leads to release of cholecystokinin a hormone important for gall bladder contraction, pancreatic enzyme secretion and gastric emptying (Wang et al., 2011). CaSR expression in the acinar cells of the pancreas and in pancreatic duct cells suggests a role for the receptor in fluid secretion and/or the secretion of enzymes from the pancreas (Racz et al., 2002; Riccardi and Kemp, 2012). The proper regulation of fluid secretion from the pancreatic ducts by the CaSR is thought to be important in the prevention of pancreatic stones and pancreatitis (Riccardi and Kemp, 2012). In addition, activation of the CaSR expressed in the β-cells of the pancreatic islets of Langerhans can modulate insulin secretion and this has implications for the onset and progression of diabetes (Gray et al., 2006; Squires et al., 2000). CaSR expression in colonic epithelial cells is required for the transition of cells along the crypt from a proliferative to a differentiated state, thus the presence of receptor in these cells is thought to be important in preventing colon cancer (Whitfield, 2009). Agonist activation of the CaSR in the colon can suppress cAMP-mediated fluid loss and is important in the control of NaCl and water absorption (Geibel and Hebert, 2009). It has been proposed that calcimimetics could be used to prevent diarrhoea/fluid loss associated with bacterial toxins in diseases such as cholera (Geibel et al., 2006).
In the lactating breast, expression of the CaSR in mammary epithelial cells can regulate parathyroid hormone-related protein (PTHrP) production and adjust uptake of calcium into milk according to calcium availability (VanHouten et al., 2004). In the normal breast the CaSR has tumour suppressor properties acting in concert with the BRCA1 tumour suppressor to decrease levels of the antiapoptotic protein, survivin, and increase sensitivity to paclitaxel, a drug commonly used in breast cancer treatment (Promkan et al., 2011). However, if expressed in malignant breast cells, the receptor may actually aid bone metastasis (see below under hypercalcaemia of malignancy). With relevance to its apparent role in metastasis, the CaSR has been shown to couple to integrins thereby promoting tumour cell adhesion and migration (Tharmalingham et al., 2011). The CaSR can also bind the focal adhesion protein, testin, that is known to have important effects on cell spreading and motility (Magno et al., 2011a).
In the brain, The CaSR is highly expressed in the subfornical organ and potentiates neuronal, hyperpolarization-activated inward currents, consistent with the bursting of action potentials in these neurons that has also been shown to be CaSR-potentiated (Washburn et al., 2000; Yano et al., 2004). The expression of the CaSR in the subfornical organ, which is a thirst control centre, suggests that the receptor plays a crucial role in fluid and electrolyte homeostasis. The CaSR also controls neuronal excitability in a number of other parts of the brain by regulating ion channels and this may contribute to its apparent role in epilepsy (Kapoor et al., 2008; Riccardi and Kemp, 2012). For example, in the hippocampus, CaSR-mediated activation of a voltage-independent Na+ leak conductance channel leads to neuronal excitation (Lu et al., 2010). In the hippocampus, increasing expression of the CaSR during the first weeks of life correlate with long-term potentiation indicating that the CaSR may play a role in cognitive functions such as memory and learning (Brown and MacLeod, 2001; Yano et al., 2004). The CaSR has important regulatory effects on the developing nervous system, for example, activation of the CaSR appears to be critical for the expansion and differentiation of oligodendrocyte progenitor cells and the generation of myelin in preoligodendrocytes (Chattopadhyay et al., 2008). Stimulation of CaSR is required for the production of a cofactor, tetrahydrobiopterin, essential for the activation of nitrous oxide that is produced (in its inactive form) in response to amyloid β peptide-mediated activation of the receptor (Dal Pra et al., 2005). Hence, CaSR may play an important role in late onset Alzheimers disease that is characterized by nitrous oxide-mediated neuronal damage. In the pituitary gland, activation of the CaSR stimulates cAMP production via coupling to Gαs with subsequent secretion of PTHrP and ACTH (Mamillapalli and Wysolmerski, 2010).
The CaSR is expressed and plays a functionally important role in various bone cells including osteoblasts/osteocytes and osteoclasts and their precursors, bone marrow derived stromal cells, monocyte-macrophage cells, chondrocytes and haematopoietic stem cells (Yamaguchi, 2008). Targeted depletion of the CaSR induced in mouse embryonic chondrocytes and osteoblasts has revealed that the CaSR is absolutely required for growth plate and skeletal development (Chang et al., 2008). Activation of the CaSR in osteoblasts is required for osteoblast differentiation, proliferation and mineralization (Yamaguchi, 2008; Dvorak-Ewell et al., 2011). In addition, high Ca2+-induced apoptosis of osteoclasts is mediated through nuclear translocation of NF-κB which in turn is dependent on CaSR stimulation and activation of PLC (Mentaverri et al., 2006). The CaSR also appears to be important in osteoclastogenesis as shown in studies with bone marrow cells from CaSR knockout mice (Dvorak-Ewell et al., 2011). The CaSR is required for haemopoietic stem cells to lodge in the endosteal niche of the bone marrow - this has implications for the proper functioning of erythropoiesis (Adams et al., 2006). The CaSR appears to contribute, albeit indirectly, to the formation of teeth and the development of dental alveolar bone (Sun et al., 2010).
The CaSR also has established roles in other organs and tissues including the heart and circulatory system. In the heart, the receptor can augment angiotensin II-mediated cardiac hypertrophy in cardiomyocytes, while CaSR-mediated production of nitrous oxide can lead to vasodilation in human aortic epithelial cells with subsequent effects on blood pressure (Ziegelstein et al., 2006; Wang et al., 2008). The CaSR has also been shown to mediate the cardio-protective effects of ischaemic preconditioning (Sun and Murphy, 2010). Expression of the CaSR in vascular smooth muscle cells of human arteries appears to be important in preventing arterial calcification (Alam et al., 2009). The CaSR appears to play an important role in the differentiation of keratinocytes and their survival (Tu et al., 2008). Lens epithelial cells express CaSR mRNA and protein and stimulation of the receptor regulates a calcium-activated potassium channel - it is likely that the receptor contributes to lens integrity (Chattopadhyay et al., 1997; Brown and MacLeod, 2001).
The receptor also has functional effects on reproduction and development (Riccardi and Kemp, 2012). The CaSR is expressed in ovarian surface cells and ova (where it is important for development and maturation), sperm (where it is important for maturation, motility and fertilization) and uterus (where it plays roles in implantation and embryonic development). Hence its proper expression has important implications for fertility. In addition the receptor plays a critical role in the placenta and in embryonic and foetal development of organs such as the lung, brain and nervous system (Riccardi and Kemp, 2012).
Homology
The human and bovine CaSR share significant homology (greater than 90% at the amino acid level) with CaSRs from other mammals such as rodents, rabbits and cats (Garrett et al., 1995; Brown and MacLeod, 2001; Gal et al., 2010). Even CaSRs from chickens and the mudpuppy (an amphibian) share approximately 80% amino acid identity underscoring the functional importance of this receptor throughout the animal kingdom (Brown and MacLeod, 2001). The CaSR belongs to Family C of the G protein-coupled receptors, members of which share at least 20% amino acid homology in their seven transmembrane domains (Brauner-Osborne et al., 2007). Group I of Family C comprise the metabotropic glutamate receptors (mGluR 1-8) whereas the CaSR belongs to Group II which also contains the vomeronasal and taste and odorant receptors and various orphan receptors including GPRC6A (the most closely related to the CaSR). Group III comprises the gammabutyric acid (GABAB) receptors). Interestingly, the CaSR can heterodimerize with mGluR and GABAB receptors resulting in receptor units with unique pharmacological profiles (Gama et al., 2001; Cheng et al., 2007). The ECD including the VFT of the Family C GPCRs shares homology with bacterial periplasmic nutrient-binding proteins (PBPs) and Family C GPCRs are thought to have evolved from fusion of an ancient PBP-like structure (forming the ECD) with an independently derived seven transmembrane domain entity (Brown and Macleod, 2001).
Mutations
Note
Heterozygous, germinal mutations in the CaSR may be activating or inactivating leading to the familial conditions of altered calcium sensing, autosomal dominant hypocalcaemia (ADH) and familial hypocalciuric hypercalcaemia (FHH), respectively (Pollak et al., 1993; Pollak et al., 1994). These disorders are usually benign and may often be asymptomatic, although in rare cases severe activating mutations of the CaSR may give rise to Bartters syndrome subtype IV (Vargas-Poussou et al., 2002). On the other hand, the homozygous presence of inactivating mutations or compound heterozygous mutations affecting both alleles of the CaSR gene give rise to the rare, but much more serious condition, neonatal severe hyperparathyroidism (NSHPT), that normally requires surgical intervention (usually sub-total parathyroidectomy) in the neonate (Pollak et al., 1993; Ward et al., 2004; Ward et al., 2012). Reported mutations leading to ADH and FHH/NSHPT number around 65 and 140, respectively and may occur almost anywhere in the CaSR gene coding region, although there is a particular preponderance in exons 3 and 4 which encode part of the extracellular ligand-binding domain that includes the VFT, and the 5 end of exon 7 which encodes the seven transmembrane, signalling domain, including the extra- and intracellular loops (Hendy et al., 2009 and see database: CASRdb).
Implicated in
Entity name
Primary and secondary hyperparathyroidism
Note
Primary hyperparathyroidism (PHPT) is most commonly caused by a single adenomatous parathyroid gland, although it can occasionally arise from double adenomas or hyperplasia of all four glands. The condition arises from suppression of the Ca2+-induced negative feedback mechanism that controls PTH secretion - essentially there is a higher set point for Ca2+-induced inhibition of PTH secretion (Cetani et al., 2000). Unlike the inherited disorders of calcium homeostasis described in the above section, CaSR mutations have not been associated with the adenomas that give rise to PHPT, rather mutations in other genes such as the MEN1 tumour suppressor and cyclin D1 oncogene predominate (Hosokawa et al., 1995; Sharretts and Simonds, 2010). However, adenomas associated with PHPT have been shown to express low levels of CaSR compared to normal parathyroid tissue (Kifor et al., 1996; Ward et al., 2012). While the reason for this reduced expression is unclear, it does lead to an exacerbation of the condition since the CaSR contributes to the altered set point for PTH release. In addition, there is further evidence for the involvement of the CaSR in PHPT: impaired CaSR-mediated amino acid sensing (as well as calcium sensing) can cause loss of negative feedback of PTH release (Mun et al., 2009) and specific allosteric activators of the CaSR (calcimimetics) have been used successfully in the treatment of PHPT (Peacock et al., 2009). Finally, various polymorphisms in the CaSR gene or its regulatory region have been linked to PHPT and/or the severity of its clinical manifestations (reviewed in Ward et al., 2012). Secondary hyperparathyroidism (SHPT) which most commonly arises from chronic kidney disease (CKD) is controlled by the CaSR as well as other factors that regulate calcium and phosphate homeostasis (Rodriguez et al., 2005b, Ward et al., 2012). Essentially, in CKD, decreased phosphate excretion and decreased output of 1,25-dihydroxyvitamin D (leading to decreased intestinal Ca2+ absorption) and skeletal resistance to PTH, result in hypocalcaemia which, through activation of the CaSR, leads to increased secretion of PTH (note that a decrease in both phosphate excretion and vitamin D production may also directly lead to increased PTH secretion). Parathyroid gland hyperplasia may then develop, leading to decreased expression of CaSR and further exacerbation of the hyperparathyroidism. As for PHPT, a rise in set point for Ca2+-induced control of PTH suppression occurs making SHPT amenable to treatment with calcimimetics (Cunningham et al., 2011).
Entity name
Hypercalcaemia of malignancy
Note
The CaSR plays a central role in hypercalcaemia of malignancy through the capacity of malignant cells expressing the CaSR to secrete PTHrP in response to agonist stimulation of the receptor (for reviews see Chattopadhyay, 2006, Ward et al., 2012). PTHrP acts like PTH to stimulate bone resorption and renal calcium reabsorption generating high Ca2+ concentrations which further stimulate the CaSR to secrete PTHrP, creating a vicious cycle. There are two types of hypercalcaemia resulting from malignancy, osteolytic hypercalcaemia and humoral hypercalcaemia (HHM), the former associated with bony metastases that act to directly resorb bone and the latter with solid tumours that secrete circulating factors that act to increase bone resorption. CaSR activation has been demonstrated to stimulate PTHrP in both breast and prostate cancer cell lines that metastasize to bone as well as in various solid tumours which are known to be associated with HHM: H-500 rat Leydig testicular cancer cells, a human lung squamous cell carcinoma cell line and a human pancreatic cell line, (FA-6) (Sanders et al., 2000; Sanders et al., 2001; Tfelt-Hansen, 2003; Morgan et al., 2006; Lorch et al., 2011). Expression of the CaSR appears to be an important predisposing factor for the generation and continued growth of bony metastases. Both breast and prostate cancer cells that express the CaSR at high levels have a greater tendency to metastasize to bone than those that express the receptor at low levels (Liao et al., 2006; Mihai et al., 2006). High Ca2+ concentrations act as a chemoattractant for breast cancer cells and this CaSR-dependent response positively correlates with the in vivo metastatic potential of several breast cancer cell lines (Saidak et al., 2009). In addition, high Ca2+ at bony metastases signalling through the CaSR may stimulate further growth of malignant cells, for example by activation of choline kinase and production of phosphocholine (Huang et al., 2009 ) or by regulating estrogen receptor-α expression and activity (Journe et al., 2004). In the prostate cancer cell line, PC-3, knockdown of the CaSR blocked Ca2+-enhanced proliferation and reduced metastatic progression in an athymic mouse model while Ca2+ stimulation enhanced PC-3 cell attachment, a critically important step in metastasis (Liao et al., 2006).
Entity name
Breast cancer
Note
Increased dietary calcium has been shown to be protective against the development of breast cancer (Negri et al., 1996) and by contrast to the CaSRs positive role in breast cancer metastasis, the CaSR in general plays a tumour suppressor role in the development of breast cancer. This apparent paradox may best be explained by differences in the properties of primary as opposed to metastasing breast cancer cells (Ward et al., 2012). Agonist activation of the CaSR in breast cancer cells down-regulates cell proliferation, cell invasion and anchorage-independent growth as well as expression of the anti-apoptotic protein, survivin, and affords an increase in sensitivity to paclitaxel, an important drug used in the treatment of breast cancer (Liu et al., 2009a). Interestingly, the BRCA1 tumour suppressor gene which mimics these effects in breast cancer cells has been shown to do this by regulating the expression of the CaSR and therefore its effect on survivin expression and paclitaxel sensitivity (Promkan et al., 2011).
Entity name
Colon cancer
Note
As for breast cancer, calcium has been shown to be chemopreventative for colon cancer with high levels being inhibitory and low levels favourable to human colonic cell proliferation (Lipkin, 1999, Kallay et al., 2000). Moreover, the CaSR is expressed in human colonocytes and has been shown to mediate these proliferative events (Kallay et al., 2000; Kallay et al., 2003). This becomes significant within the colonic crypts where a concentration gradient which increases from the base to the apex of the crypt allows for early proliferation of stem cells at the base of the crypt and their subsequent differentiation to functional colonic epithelial cells and finally their apoptogenesis at the apex of the crypt (reviewed by Whitfield, 2009; Ward et al., 2012). This process is regulated in part by the CaSR which is expressed in cells in response to calcium as they move up the crypt. In turn, stimulation of the CaSR signals cells to stop dividing and start differentiating. This occurs primarily by CaSR-mediated suppression of components of the wnt signalling pathway such as β-catenin/TCF-4 which control nuclear cell cycle activators such as c-myc and cyclin D1 (Chakrabarty et al., 2003; Whitfield, 2009). CaSR stimulation also produces E-cadherin which links up with β-catenin to form adherens junctions allowing cell-cell connections and at the same time sequestering β-catenin away from the nucleus (Bhagavathula et al., 2007). CaSR stimulation also leads to increased expression of the cyclin-dependent kinase inhibitors, p21 and p27, and down-regulates expression of the anti-apoptotic protein, survivin (Chakrabarty et al., 2005; Liu et al., 2009b). Taken together, it has been concluded that low levels of Ca2+ in the colon and/or a poorly expressed or functionally compromised CaSR could lead to a lack of control of cell proliferation in colonic crypt development leading to potential malignancy (Whitfield, 2009; Ward et al., 2012).
Entity name
Pancreatitis
Note
Chronic pancreatitis develops largely as a result of a build-up of trypsin resulting in tissue injury and inflammation. Hypercalcaemia associated with inactivating mutations of the CaSR might be expected to lead to high exposure of pancreatic acinar cells to Ca2+ leading to the activation of trypsinogen to trypsin and a reduction in chymotrypsin C-mediated degradation of trypsin (Racz et al., 2002; Whitcomb, 2010). Although inactivating CaSR mutations are sometimes associated with pancreatitis, no causal link between CASR/FHH and pancreatitis could be demonstrated (Stuckey et al., 1990; Pearce et al., 1996). However, there is a stronger association between concurrent mutations in the SPINK1 and CaSR genes and pancreatitis (reviewed by Whitcomb, 2010). The SPINK1 gene encodes a protein (serine protease inhibitor Kazal 1) that blocks trypsin in response to tissue inflammation. The current belief is that neither CASR nor SPINK1 gene mutations act alone to cause pancreatitis but together and/or in association with other factors appear to contribute to the pathogenesis of this disease (Whitcomb, 2010).
Entity name
Cardiovascular disease/hypertension
Note
There is mounting evidence that the CaSR plays an important role in the regulation of blood pressure. Stimulation of human aortic epithelial cells with spermine enhanced the production of nitrous oxide and this effect was prevented by siRNA- specific targeting of the CaSR, strongly suggesting a role for the receptor in vasodilation (Ziegelstein et al., 2006). In addition, activation of the CaSR expressed in the juxtaglomerular cells of the afferent arteriole of the kidney inhibits release of renin, thus exerting influence over the renin-angiotensin system that controls blood pressure (Atchison et al., 2010). Further to this, angiotensin II stimulates cardiac hypertrophy and this results in increased expression of the CaSR in the cardiomyocytes which, when activated, further drives angiotensin II-mediated hypertrophy (Wang et al., 2008; Magno et al., 2011b). The CaSR may also contribute to cardiac hypertrophy by IP3-mediated increases in nuclear Ca2+ and engagement of the CaN/NFAT pathway (Zhong et al., 2012). External stresses such as hypoxia-reoxygenation, ischaemia-reperfusion and the application of atherogenic agents have also been shown to increase CaSR expression in cardiac myocytes (reviewed in Magno et al., 2011b). Interestingly, the CaSR has been demonstrated to mediate the cardio-protective effects of ischaemic preconditioning (Sun and Murphy, 2010). The CaSR is also expressed in vascular smooth muscle cells of human arteries where its increased activation is associated with decreased mineralization (Alam et al., 2009). This is consistent with reduced expression of the CaSR in the atherosclerotic, highly calcified arteries found in patients with hypercalcaemia associated with secondary hyperparathyroidism and end stage CKD (Alam et al., 2009; Cunningham et al., 2011).
Entity name
Brain disease
Note
The CaSR is implicated to play a role in Alzheimers disease (AD), with polymorphisms in intron 4 and exon 7 of the CaSR linked to AD status (Conley et al., 2009). Both amyloid-β peptide as well as apolipoprotein E protein can activate the CaSR with the former shown to have effects on calcium permeable, non-selective cation channels in hippocampal pyramidal neurons (Ye et al., 1997; Conley et al., 2009). Nitrous oxide is responsible for the neuronal cell death characterizing late onset AD and the CaSR is necessary for the generation of a cofactor (tetrahydrobiopterin) important in the activation of nitrous oxide that is produced (in its inactive form) in response to amyloid-β peptide-mediated stimulation of the receptor (Dal Pra et al., 2005; Chiarini et al., 2009). The CaSR has also been linked to other brain diseases such as epilepsy with a mutation in the CaSR (R898Q) reported to cosegregate with idiopathic epilepsy in a family from Southern India (Kapoor et al., 2008). The CaSR appears to be critical for the expression of mRNA for myelin basic protein in preoligodendrocytes and therefore for proper myelination (Chattopadhyay et al., 2008) - in this respect it is likely that a non-functional CaSR could lead to impaired neurodevelopment.
Entity name
Bone disease
Note
The CaSR is expressed in osteoblasts/osteocytes and osteoclasts and their precursors, bone marrow derived stromal cells, monocyte-macrophage cells, chondrocytes and haematopoietic stem cells (reviewed by Yamaguchi, 2008). Expression of a functional CaSR is critical for growth plate development/endochronal bone formation, postnatal bone development and osteoblast differentiation and the effects on these processes are independent of CaSR-mediated PTH secretion (Brown and Lian, 2008; Chang et al., 2008; Dvorak-Ewell et al., 2011). The CaSR also appears to be important postnatally for proper teeth and dental alveolar bone formation (Sun et al., 2010) and upregulation of the CaSR in chondrocytes may contribute to the progression of osteoarthritis (Burton et al., 2005). While the CaSR has not been linked to the development of osteoporosis, therapeutic agents such as strontium ranelate and calcilytic compounds which act through the CaSR have been used or proposed for its treatment (Trivedi et al., 2010; Marie et al., 2011).
Entity name
Other disease associations
Note
Activation of the CaSR expressed in the β-cells of the islets of Langerhans of the pancreas can modulate insulin secretion and hence the receptor may play a role in diabetes mellitus (Gray et al., 2006; Squires et al., 2000). For example, L-histidine activation of the CaSR appears to negatively modulate glucose-induced insulin secretion from β-cells through changes in spatial arrangement of the CaSR and L-type voltage-dependent calcium channels that are important for Ca2+-dependent triggering of insulin release (Parkash and Asotra, 2011). Amino acid activation of the CaSR expressed in the I cells of the duodenum results in secretion of the hormone, cholecystokinin, which is important for the regulation of gall bladder contraction, pancreatic function, gastric emptying and satiety with the latter two having implications for obesity (Wang et al., 2011). In the kidney, proper regulation of AQP2 water channels and vacuolar H+-ATPase through activation of the CaSR in the collecting ducts is important for preventing kidney stones (Sands et al., 1998; Procino et al., 2004; Riccardi and Kemp, 2012) and stimulation of the CaSR expressed in podocytes of the Bowmans capsule of the kidney glomerulus, helps maintain their cytoskeletal integrity and overall survival thus preventing glomerular disease including proteinuria (Oh et al., 2011).
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 16382241 | 2006 | Stem cell engraftment at the endosteal niche is specified by the calcium-sensing receptor. | Adams GB et al |
| 18852253 | 2009 | Calcification is associated with loss of functional calcium-sensing receptor in vascular smooth muscle cells. | Alam MU et al |
| 20660105 | 2010 | Acute activation of the calcium-sensing receptor inhibits plasma renin activity in vivo. | Atchison DK et al |
| 10077597 | 1999 | Intermolecular interactions between dimeric calcium-sensing receptor monomers are important for its normal function. | Bai M et al |
| 17557293 | 2007 | Regulation of E-cadherin and beta-catenin by Ca2+ in colon carcinoma is dependent on calcium-sensing receptor expression and function. | Bhagavathula N et al |
| 12605346 | 2003 | Signaling of the human calcium-sensing receptor expressed in HEK293-cells is modulated by protein kinases A and C. | Bösel J et al |
| 17266540 | 2007 | Structure, pharmacology and therapeutic prospects of family C G-protein coupled receptors. | Bräuner-Osborne H et al |
| 19355937 | 2009 | Regulation of cellular signal transduction pathways by the extracellular calcium-sensing receptor. | Brennan SC et al |
| 8255296 | 1993 | Cloning and characterization of an extracellular Ca(2+)-sensing receptor from bovine parathyroid. | Brown EM et al |
| 18765829 | 2008 | New insights in bone biology: unmasking skeletal effects of the extracellular calcium-sensing receptor. | Brown EM et al |
| 11152759 | 2001 | Extracellular calcium sensing and extracellular calcium signaling. | Brown EM et al |
| 15882563 | 2005 | Chondrocyte calcium-sensing receptor expression is up-regulated in early guinea pig knee osteoarthritis and modulates PTHrP, MMP-13, and TIMP-3 expression. | Burton DW et al |
| 15684428 | 2005 | Calcium-sensing receptor gene transcription is up-regulated by the proinflammatory cytokine, interleukin-1beta. Role of the NF-kappaB PATHWAY and kappaB elements. | Canaff L et al |
| 18712808 | 2009 | Glial cells missing-2 (GCM2) transactivates the calcium-sensing receptor gene: effect of a dominant-negative GCM2 mutant associated with autosomal dominant hypoparathyroidism. | Canaff L et al |
| 11134144 | 2000 | Parathyroid expression of calcium-sensing receptor protein and in vivo parathyroid hormone-Ca(2+) set-point in patients with primary hyperparathyroidism. | Cetani F et al |
| 15695391 | 2005 | Calcium sensing receptor in human colon carcinoma: interaction with Ca(2+) and 1,25-dihydroxyvitamin D(3). | Chakrabarty S et al |
| 18765830 | 2008 | The extracellular calcium-sensing receptor (CaSR) is a critical modulator of skeletal development. | Chang W et al |
| 18438915 | 2008 | Calcium receptor expression and function in oligodendrocyte commitment and lineage progression: potential impact on reduced myelin basic protein in CaR-null mice. | Chattopadhyay N et al |
| 17615148 | 2007 | Type B gamma-aminobutyric acid receptors modulate the function of the extracellular Ca2+-sensing receptor and cell differentiation in murine growth plate chondrocytes. | Cheng Z et al |
| 19355942 | 2009 | Calcium-sensing receptor (CaSR) in human brain's pathophysiology: roles in late-onset Alzheimer's disease (LOAD). | Chiarini A et al |
| 10713061 | 2000 | Cloning and characterization of two promoters for the human calcium-sensing receptor (CaSR) and changes of CaSR expression in parathyroid adenomas. | Chikatsu N et al |
| 17030896 | 2006 | Taste receptors in the gastrointestinal tract. II. L-amino acid sensing by calcium-sensing receptors: implications for GI physiology. | Conigrave AD et al |
| 19035514 | 2009 | Evidence supporting a role for the calcium-sensing receptor in Alzheimer disease. | Conley YP et al |
| 21454719 | 2011 | Secondary hyperparathyroidism: pathogenesis, disease progression, and therapeutic options. | Cunningham J et al |
| 16052472 | 2005 | Roles of Ca2+ and the Ca2+-sensing receptor (CASR) in the expression of inducible NOS (nitric oxide synthase)-2 and its BH4 (tetrahydrobiopterin)-dependent activation in cytokine-stimulated adult human astrocytes. | Dal Pra I et al |
| 21956637 | 2011 | Osteoblast extracellular Ca2+ -sensing receptor regulates bone development, mineralization, and turnover. | Dvorak-Ewell MM et al |
| 19474191 | 2009 | The full-length calcium-sensing receptor dampens the calcemic response to 1alpha,25(OH)2 vitamin D3 in vivo independently of parathyroid hormone. | Egbuna O et al |
| 11489900 | 2001 | Heterodimerization of calcium sensing receptors with metabotropic glutamate receptors in neurons. | Gama L et al |
| 7759551 | 1995 | Molecular cloning and functional expression of human parathyroid calcium receptor cDNAs. | Garrett JE et al |
| 16760252 | 2006 | Calcium-sensing receptor abrogates secretagogue- induced increases in intestinal net fluid secretion by enhancing cyclic nucleotide destruction. | Geibel J et al |
| 19575679 | 2009 | The functions and roles of the extracellular Ca2+-sensing receptor along the gastrointestinal tract. | Geibel JP et al |
| 22114145 | 2011 | Agonist-driven maturation and plasma membrane insertion of calcium-sensing receptors dynamically control signal amplitude. | Grant MP et al |
| 17003271 | 2006 | Activation of the extracellular calcium-sensing receptor initiates insulin secretion from human islets of Langerhans: involvement of protein kinases. | Gray E et al |
| 20374733 | 2009 | Calcium-sensing receptor and associated diseases. | Hendy GN et al |
| 7593409 | 1995 | Mutational analysis of the extracellular Ca(2+)-sensing receptor gene in human parathyroid tumors. | Hosokawa Y et al |
| 12890593 | 2003 | Naturally occurring mutations of the extracellular Ca2+-sensing receptor: implications for its structure and function. | Hu J et al |
| 19716891 | 2009 | Activation of choline kinase by extracellular Ca2+ is Ca(2+)-sensing receptor, Galpha12 and Rho-dependent in breast cancer cells. | Huang C et al |
| 8597637 | 1995 | Mapping of the calcium-sensing receptor gene (CASR) to human chromosome 3q13.3-21 by fluorescence in situ hybridization, and localization to rat chromosome 11 and mouse chromosome 16. | Janicic N et al |
| 15268900 | 2004 | Extracellular calcium downregulates estrogen receptor alpha and increases its transcriptional activity through calcium-sensing receptor in breast cancer cells. | Journé F et al |
| 17962359 | 2008 | The extracellular calcium-sensing receptor (CaSR) on human esophagus and evidence of expression of the CaSR on the esophageal epithelial cell line (HET-1A). | Justinich CJ et al |
| 10917132 | 2000 | Dietary calcium and growth modulation of human colon cancer cells: role of the extracellular calcium-sensing receptor. | Kállay E et al |
| 12899245 | 2003 | Molecular and functional characterization of the extracellular calcium-sensing receptor in human colon cancer cells. | Kállay E et al |
| 18756473 | 2008 | An idiopathic epilepsy syndrome linked to 3q13.3-q21 and missense mutations in the extracellular calcium sensing receptor gene. | Kapoor A et al |
| 9705306 | 1998 | The calcium-sensing receptor is localized in caveolin-rich plasma membrane domains of bovine parathyroid cells. | Kifor O et al |
| 8636374 | 1996 | Reduced immunostaining for the extracellular Ca2+-sensing receptor in primary and uremic secondary hyperparathyroidism. | Kifor O et al |
| 16982748 | 2006 | Extracellular calcium as a candidate mediator of prostate cancer skeletal metastasis. | Liao J et al |
| 10668488 | 1999 | Preclinical and early human studies of calcium and colon cancer prevention. | Lipkin M et al |
| 18618519 | 2009 | Calcium and calcium sensing receptor modulates the expression of thymidylate synthase, NAD(P)H:quinone oxidoreductase 1 and survivin in human colon carcinoma cells: promotion of cytotoxic response to mitomycin C and fluorouracil. | Liu G et al |
| 21532883 | 2011 | The calcium-sensing receptor is necessary for the rapid development of hypercalcemia in human lung squamous cell carcinoma. | Lorch G et al |
| 21040849 | 2010 | Extracellular calcium controls background current and neuronal excitability via an UNC79-UNC80-NALCN cation channel complex. | Lu B et al |
| 21843504 | 2011 | Testin, a novel binding partner of the calcium-sensing receptor, enhances receptor-mediated Rho-kinase signalling. | Magno AL et al |
| 20729338 | 2011 | The calcium-sensing receptor: a molecular perspective. | Magno AL et al |
| 20032198 | 2010 | The calcium-sensing receptor couples to Galpha(s) and regulates PTHrP and ACTH secretion in pituitary cells. | Mamillapalli R et al |
| 20812008 | 2011 | How strontium ranelate, via opposite effects on bone resorption and formation, prevents osteoporosis. | Marie PJ et al |
| 17077282 | 2006 | The calcium sensing receptor is directly involved in both osteoclast differentiation and apoptosis. | Mentaverri R et al |
| 16564154 | 2006 | Expression of the calcium receptor in human breast cancer--a potential new marker predicting the risk of bone metastases. | Mihai R et al |
| 17078869 | 2006 | Calcium insensitivity of FA-6, a cell line derived from a pancreatic cancer associated with humoral hypercalcemia, is mediated by the significantly reduced expression of the Calcium Sensitive Receptor transduction component p38 MAPK. | Morgan R et al |
| 19567535 | 2009 | Adenomatous human parathyroid cells exhibit impaired sensitivity to L-amino acids. | Mun HC et al |
| 8567108 | 1996 | Intake of selected micronutrients and the risk of breast cancer. | Negri E et al |
| 9520489 | 1998 | Calcimimetics with potent and selective activity on the parathyroid calcium receptor. | Nemeth EF et al |
| 21508926 | 2011 | Stimulation of the calcium-sensing receptor stabilizes the podocyte cytoskeleton, improves cell survival, and reduces toxin-induced glomerulosclerosis. | Oh J et al |
| 19892707 | 2010 | Involvement of the calcium-sensing receptor in human taste perception. | Ohsu T et al |
| 21219913 | 2011 | L-histidine sensing by calcium sensing receptor inhibits voltage-dependent calcium channel activity and insulin secretion in β-cells. | Parkash J et al |
| 19837909 | 2009 | Cinacalcet treatment of primary hyperparathyroidism: biochemical and bone densitometric outcomes in a five-year study. | Peacock M et al |
| 9039332 | 1996 | Calcium-sensing receptor mutations in familial hypocalciuric hypercalcaemia with recurrent pancreatitis. | Pearce SH et al |
| 16740594 | 2006 | Calcium-sensing receptor dimerizes in the endoplasmic reticulum: biochemical and biophysical characterization of CASR mutants retained intracellularly. | Pidasheva S et al |
| 7874174 | 1994 | Autosomal dominant hypocalcaemia caused by a Ca(2+)-sensing receptor gene mutation. | Pollak MR et al |
| 15569313 | 2004 | Extracellular calcium antagonizes forskolin-induced aquaporin 2 trafficking in collecting duct cells. | Procino G et al |
| 21296416 | 2011 | BRCA1 suppresses the expression of survivin and promotes sensitivity to paclitaxel through the calcium sensing receptor (CaSR) in human breast cancer cells. | Promkan M et al |
| 12377811 | 2002 | Extracellular calcium sensing receptor in human pancreatic cells. | Rácz GZ et al |
| 9852126 | 1998 | Identification of the sites of N-linked glycosylation on the human calcium receptor and assessment of their role in cell surface expression and signal transduction. | Ray K et al |
| 9395465 | 1997 | The carboxyl terminus of the human calcium receptor. Requirements for cell-surface expression and signal transduction. | Ray K et al |
| 22017175 | 2012 | The calcium-sensing receptor beyond extracellular calcium homeostasis: conception, development, adult physiology, and disease. | Riccardi D et al |
| 18096993 | 2008 | Destabilization of parathyroid hormone mRNA by extracellular Ca2+ and the calcimimetic R-568 in parathyroid cells: role of cytosolic Ca and requirement for gene transcription. | Ritter CS et al |
| 16166224 | 2005 | Expression and functional assessment of an alternatively spliced extracellular Ca2+-sensing receptor in growth plate chondrocytes. | Rodriguez L et al |
| 15507543 | 2005 | The calcium-sensing receptor: a key factor in the pathogenesis of secondary hyperparathyroidism. | Rodriguez M et al |
| 19285978 | 2009 | Extracellular calcium promotes the migration of breast cancer cells through the activation of the calcium sensing receptor. | Saidak Z et al |
| 11701443 | 2001 | Ca(2+)-sensing receptor expression and PTHrP secretion in PC-3 human prostate cancer cells. | Sanders JL et al |
| 9612337 | 1998 | Vasopressin-elicited water and urea permeabilities are altered in IMCD in hypercalcemic rats. | Sands JM et al |
| 20833339 | 2010 | Clinical and molecular genetics of parathyroid neoplasms. | Sharretts JM et al |
| 10868962 | 2000 | The extracellular calcium-sensing receptor on human beta-cells negatively modulates insulin secretion. | Squires PE et al |
| 2285390 | 1990 | Familial hypocalciuric hypercalcaemia and pancreatitis: no causal link proven. | Stuckey BG et al |
| 20833954 | 2010 | Calcium-sensing receptor: a sensor and mediator of ischemic preconditioning in the heart. | Sun J et al |
| 20150282 | 2010 | Alterations in phosphorus, calcium and PTHrP contribute to defects in dental and dental alveolar bone formation in calcium-sensing receptor-deficient mice. | Sun W et al |
| 15697170 | 2005 | The calcium-sensing receptor in normal physiology and pathophysiology: a review. | Tfelt-Hansen J et al |
| 21969374 | 2011 | Calcium-sensing receptor modulates cell adhesion and migration via integrins. | Tharmalingam S et al |
| 20629616 | 2010 | Investigational anabolic therapies for osteoporosis. | Trivedi R et al |
| 18065418 | 2008 | Inactivation of the calcium sensing receptor inhibits E-cadherin-mediated cell-cell adhesion and calcium-induced differentiation in human epidermal keratinocytes. | Tu CL et al |
| 14966569 | 2004 | The calcium-sensing receptor regulates mammary gland parathyroid hormone-related protein production and calcium transport. | VanHouten J et al |
| 12191970 | 2002 | Functional characterization of a calcium-sensing receptor mutation in severe autosomal dominant hypocalcemia with a Bartter-like syndrome. | Vargas-Poussou R et al |
| 18295598 | 2008 | Involvement of calcium-sensing receptor in cardiac hypertrophy-induced by angiotensinII through calcineurin pathway in cultured neonatal rat cardiomyocytes. | Wang LN et al |
| 21183662 | 2011 | Amino acids stimulate cholecystokinin release through the Ca2+-sensing receptor. | Wang Y et al |
| 22503956 | 2012 | The role of the calcium-sensing receptor in human disease. | Ward BK et al |
| 11043554 | 2000 | The calcium receptor modulates the hyperpolarization-activated current in subfornical organ neurons. | Washburn DL et al |
| 20059346 | 2010 | Genetic aspects of pancreatitis. | Whitcomb DC et al |
| 18725175 | 2009 | Calcium, calcium-sensing receptor and colon cancer. | Whitfield JF et al |
| 18600395 | 2008 | The calcium-sensing receptor in bone. | Yamaguchi T et al |
| 15200149 | 2004 | Calcium-sensing receptor in the brain. | Yano S et al |
| 9067864 | 1997 | Amyloid-beta proteins activate Ca(2+)-permeable channels through calcium-sensing receptors. | Ye C et al |
| 11069904 | 2001 | The extracellular calcium-sensing receptor dimerizes through multiple types of intermolecular interactions. | Zhang Z et al |
| 22708524 | 2012 | Calcium sensing receptor regulates cardiomyocyte function through nuclear calcium. | Zhong X et al |
| 16472767 | 2006 | Expression of a functional extracellular calcium-sensing receptor in human aortic endothelial cells. | Ziegelstein RC et al |
Other Information
Locus ID:
NCBI: 846
MIM: 601199
HGNC: 1514
Ensembl: ENSG00000036828
Variants:
dbSNP: 846
ClinVar: 846
TCGA: ENSG00000036828
COSMIC: CASR
RNA/Proteins
| Gene ID | Transcript ID | Uniprot |
|---|---|---|
| ENSG00000036828 | ENST00000490131 | A0A1X7SBX3 |
| ENSG00000036828 | ENST00000498619 | P41180 |
| ENSG00000036828 | ENST00000638421 | P41180 |
| ENSG00000036828 | ENST00000639785 | P41180 |
Expression (GTEx)
Pathways
Protein levels (Protein atlas)
PharmGKB
| Entity ID | Name | Type | Evidence | Association | PK | PD | PMIDs |
|---|---|---|---|---|---|---|---|
| PA128394595 | PLCH1 | Gene | Pathway | associated | |||
| PA134875646 | PLCZ1 | Gene | Pathway | associated | |||
| PA134914471 | PLCH2 | Gene | Pathway | associated | |||
| PA164713150 | Parathyroid Hormones And Analogues | Chemical | LabelAnnotation | associated | |||
| PA33384 | PLCB1 | Gene | Pathway | associated | |||
| PA33385 | PLCB2 | Gene | Pathway | associated | |||
| PA33386 | PLCB3 | Gene | Pathway | associated | |||
| PA33387 | PLCB4 | Gene | Pathway | associated | |||
| PA33388 | PLCD1 | Gene | Pathway | associated | |||
| PA33389 | PLCD3 | Gene | Pathway | associated | |||
| PA33390 | PLCD4 | Gene | Pathway | associated | |||
| PA33391 | PLCE1 | Gene | Pathway | associated | |||
| PA33392 | PLCG1 | Gene | Pathway | associated | |||
| PA33393 | PLCG2 | Gene | Pathway | associated | |||
| PA33394 | PLCL1 | Gene | Pathway | associated | |||
| PA33395 | PLCL2 | Gene | Pathway | associated |
References
| Pubmed ID | Year | Title | Citations |
|---|---|---|---|
| 37837817 | 2024 | Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue. | 1 |
| 38285634 | 2024 | Exploring Adaptive Phenotypes for the Human Calcium-Sensing Receptor Polymorphism R990G. | 0 |
| 38326620 | 2024 | Allosteric modulation and G-protein selectivity of the Ca(2+)-sensing receptor. | 5 |
| 38561929 | 2024 | Functional evaluation of a novel nonsense variant of the calcium-sensing receptor gene leading to hypocalcemia. | 0 |
| 38632411 | 2024 | Promiscuous G-protein activation by the calcium-sensing receptor. | 0 |
| 37837817 | 2024 | Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue. | 1 |
| 38285634 | 2024 | Exploring Adaptive Phenotypes for the Human Calcium-Sensing Receptor Polymorphism R990G. | 0 |
| 38326620 | 2024 | Allosteric modulation and G-protein selectivity of the Ca(2+)-sensing receptor. | 5 |
| 38561929 | 2024 | Functional evaluation of a novel nonsense variant of the calcium-sensing receptor gene leading to hypocalcemia. | 0 |
| 38632411 | 2024 | Promiscuous G-protein activation by the calcium-sensing receptor. | 0 |
| 36626889 | 2023 | Subtotal Parathyroidectomy Successfully Controls Calcium Levels of Patients with Neonatal Severe Hyperparathyroidism Carrying a Novel CASR Mutation. | 2 |
| 36755240 | 2023 | Primary and secondary hyperparathyroidism present different expressions of calcium-sensing receptor. | 1 |
| 36786422 | 2023 | Characterizing the Role of Calcium Sensing Receptor in the Progression of Obesity-Mediated Aggressive Prostate Cancer Phenotype. | 0 |
| 36812896 | 2023 | Novel Calcium-Sensing Receptor (CASR) Mutation in a Family with Autosomal Dominant Hypocalcemia Type 1 (ADH1): Genetic Study over Three Generations and Clinical Characteristics. | 2 |
| 37060830 | 2023 | Modulation of fibroblast growth factor-23 expression and transepithelial calcium absorption in Caco-2 monolayer by calcium-sensing receptor and calcineurin under calcium hyperabsorptive state. | 0 |
Citation
Bryan Ward ; Aaron Magno ; Thomas Ratajczak
CASR (Calcium-Sensing Receptor)
Atlas Genet Cytogenet Oncol Haematol. 2013-09-01
Online version: http://atlasgeneticsoncology.org/gene/43977/casr-(calcium-sensing-receptor)
